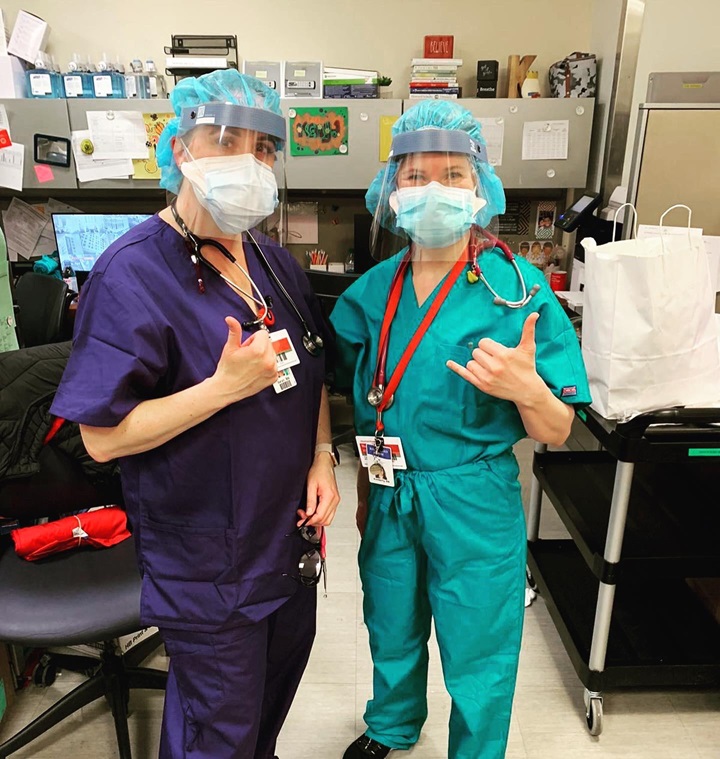
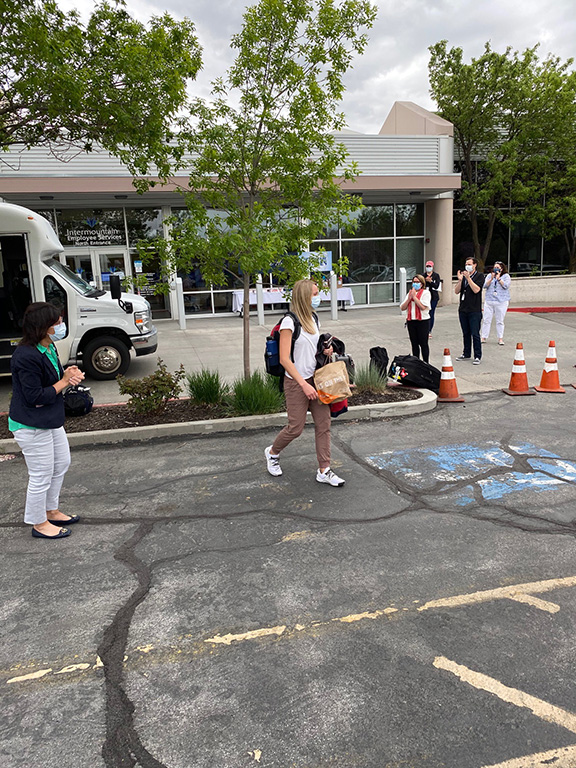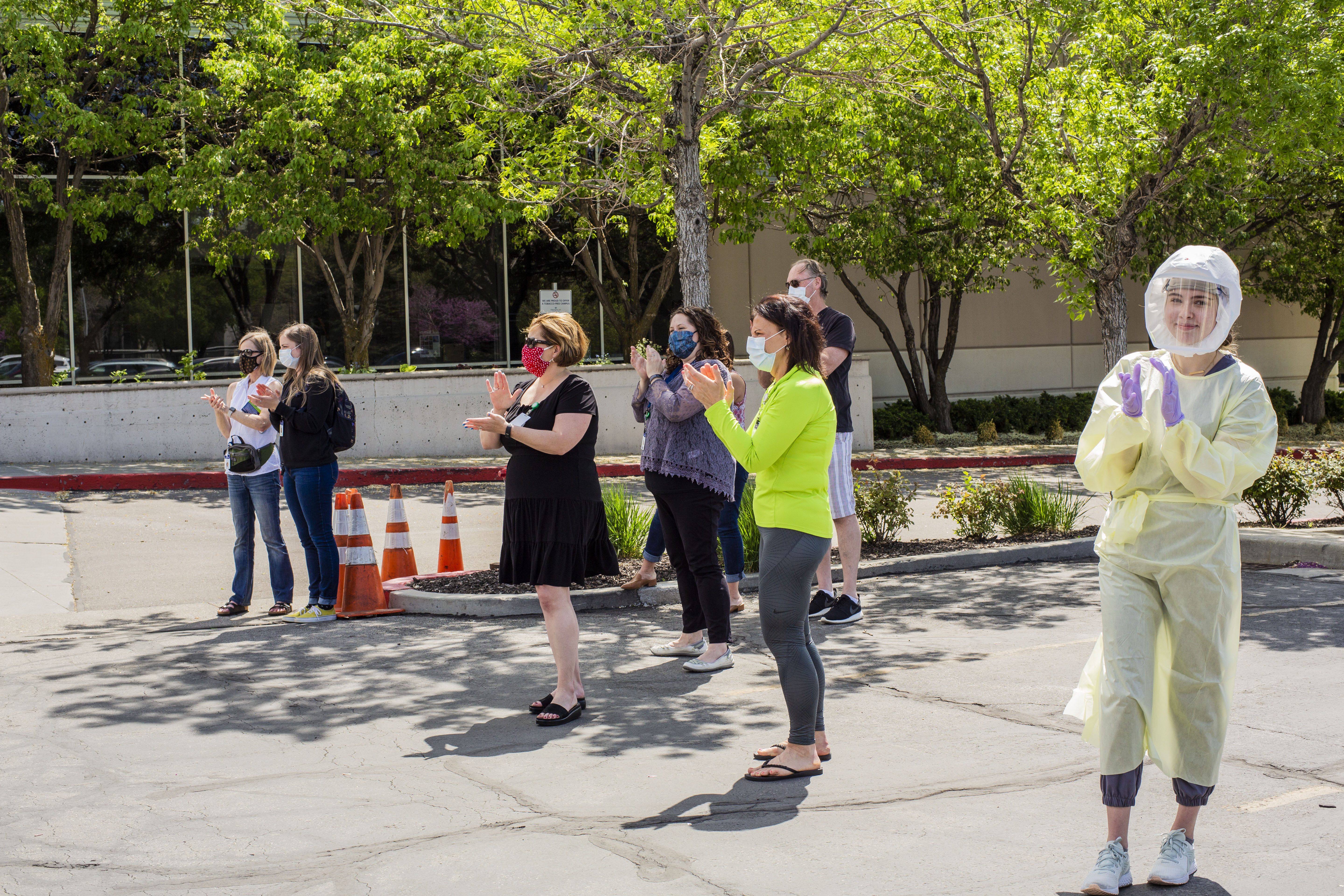Follow along as caregivers from Intermountain’s COVID-19 Response Team offer a glimpse into the COVID-19 pandemic in New York and share their experiences from the frontlines.
Intermountain Healthcare Stands with New York
Intermountain Healthcare Stands with New York
By Intermountain Health
Updated
5 minute read
Wednesday, May 27
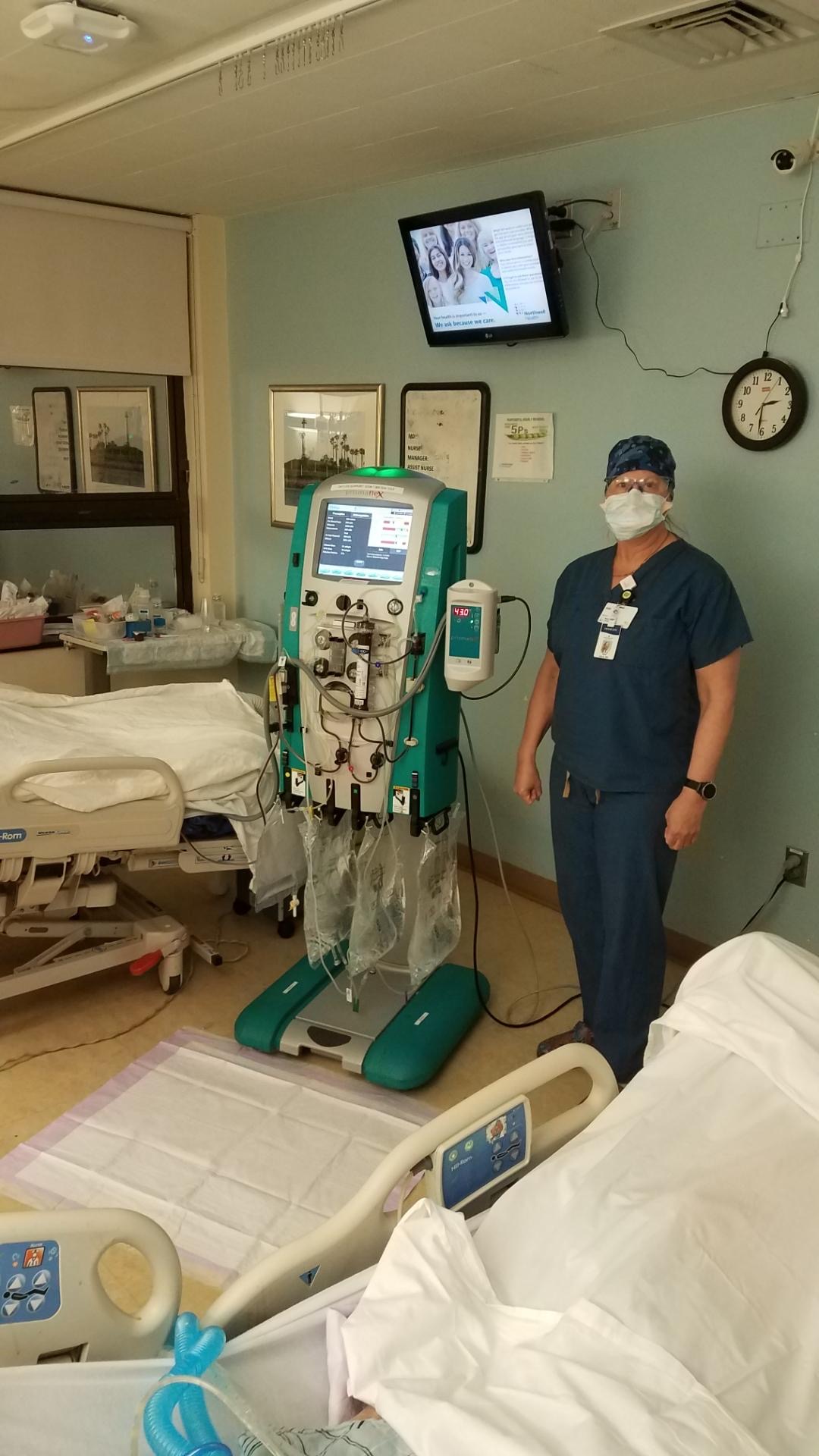
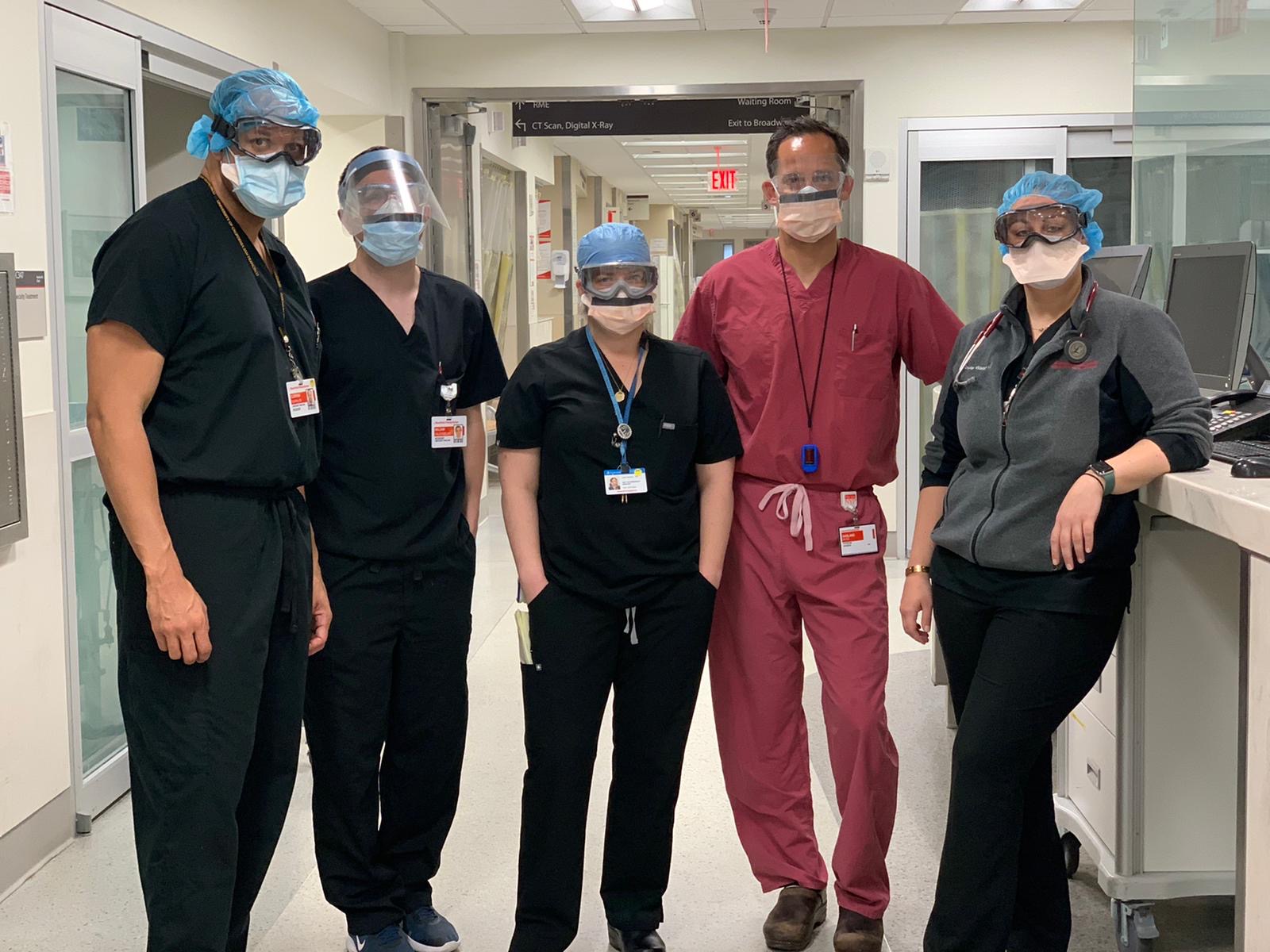
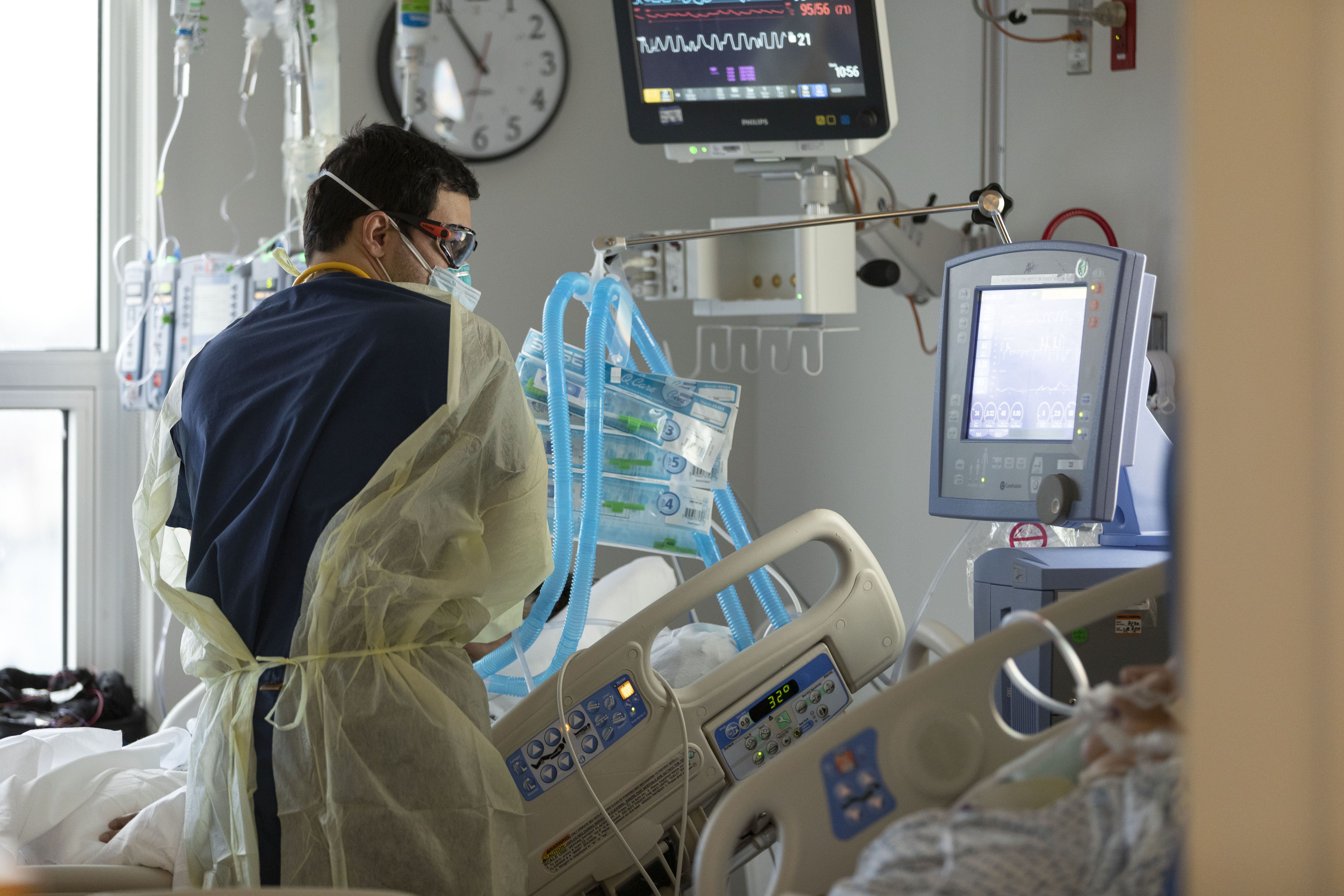
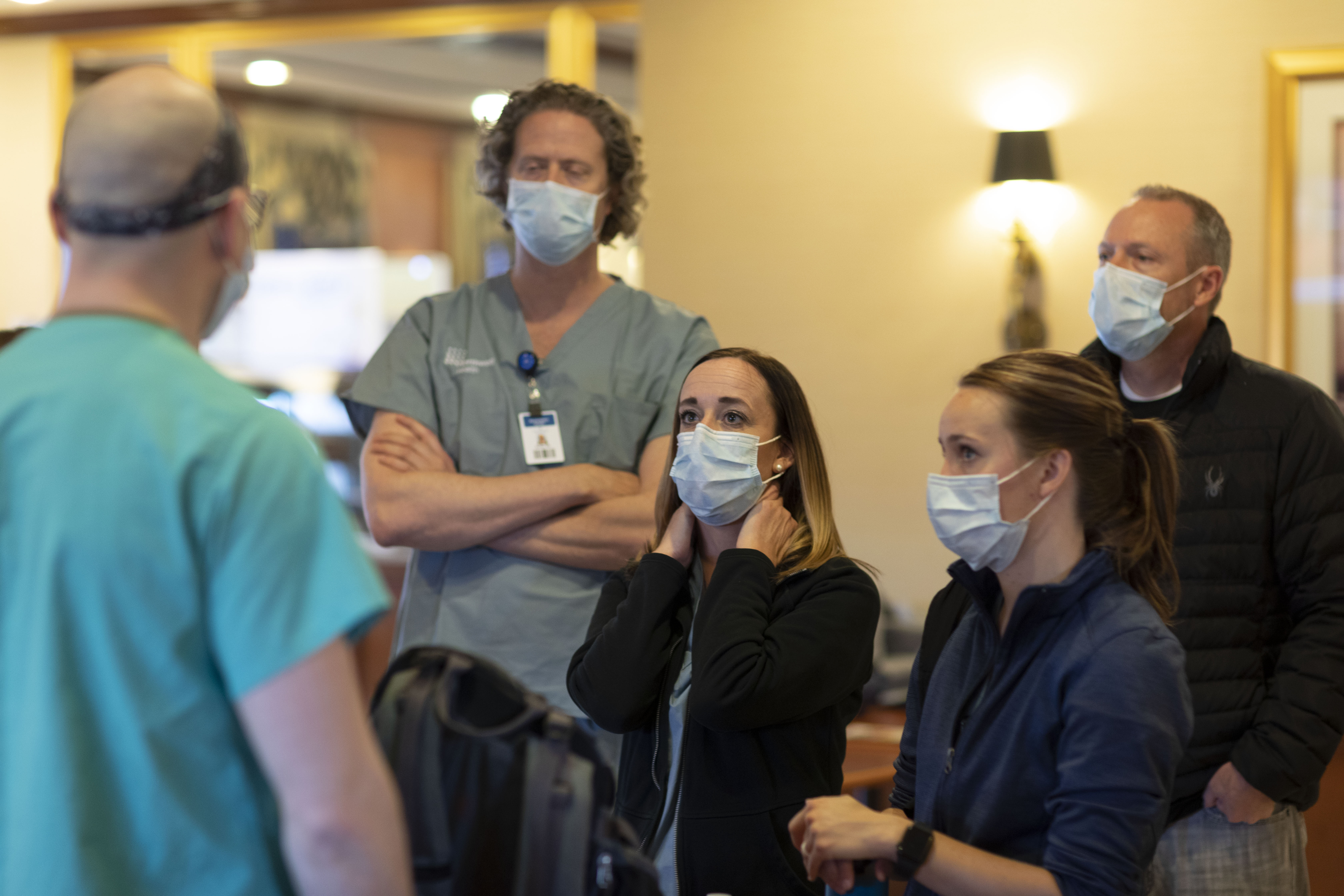
Reflections from the frontlines: Three respiratory therapists share their experiences from the pandemic frontlines.
Caregivers on Intermountain’s COVID-19 response teams continue to share stories from their deployment to the frontlines of the COVID-19 pandemic in New York. In today’s post: Respiratory therapists aren’t often in the spotlight, but their role has taken center stage during the COVID-19 because of the virus’ devastating effect on the respiratory system. Intermountain respiratory therapists Kate Wright from Alta View Hospital, Fred Ashton from Riverton Hospital, and Jesse du Toit from Intermountain Medical Center share what they experienced in New York and what they were able to bring back to their teams in Utah. In his reflection, Fred says, “Whether the New York nurses realized it or not, they’re heroes to me. I was only there for two weeks and got to come back to Utah. They’ve been there the whole time with no end in sight.”
Click to read the full story.
Friday, May 15
Reflections from the frontline: ‘COVID-19 does not discriminate.’
Sarah Jones, RN, emergency department nurse at McKay-Dee Hospital, shares her perspective after being one of 100 caregivers deployed to New York City as part of Intermountain’s COVID-19 Response Team. Sarah was at NewYork-Presbyterian Columbia Hospital.
When I got the email saying I was selected to go to NYC, I was shaking. I was so scared, but equally honored and humbled to be chosen to do what I love in a place that needed help most. I was leaving in a day and a half. Intermountain was awesome at making sure I knew I would be provided adequate PPE while there and also provided me with a big bag of PPE for travel, purple wipes, Avagard (hospital hand sanitizer), mini hand sanitizers, thank you gifts, etc.
On the plane to NYC, I made the mistake of watching the news and saw there were 606 deaths in NYC in the past 24 hours. I felt overwhelmed and scared. When we got there, we were shuttled to our hotel where we were able to get settled. The next day, the group assigned to NewYork-Presbyterian Colombia Hospital was shuttled to the campus, and we spent the day learning their POC (point of care) testing machines and IV pumps, and took a tour of the campus. The hospital was huge and took up a few blocks. It's located right next to Harlem and has 738 beds. The ED (emergency department) director told us a little about the past few weeks. Before the outbreak happened, they had 117 ICU beds. When they started to see the quick influx of vented/very sick COVID patients, they converted regular hospital beds and OR suites to make a total of 258 ICU beds in just 3 days! They informed me that their ED had 250 patients at one time, which meant doubling patient’s rooms, and finding spaces for patients in the hallways. Patient to caregiver ratios were stretched. They converted unique areas into ICUs. It was an overload of information, and I was trying to absorb it all. The next day we had a crash course on EPIC charting. I went to work my first day, shadowed a nurse for a few hours, and then was on my own. Luckily by this time, the volume was going down, so it was not as previously mentioned—but it was still very busy with very sick patients. We were able to lower patient ratios and give some nurses much needed days off. Because of the crisis levels of care this virus has caused, I had anywhere from 5 to 7 patients all while being my own phlebotomist, EKG (electrocardiography) tech, and RT (respiratory therapist). It was a lot of responsibility! I was able to meet and work with such amazing and strong nurses; I learned so much from them.
On my second day, I walked through the ED ICU, which had 17 patients at this time. I saw people who had passed away under white sheets. It was eye-opening. A few days into the workweek, the ED heard word that one of their staff, who became sick and was intubated, had passed away. It was an emotional time for the ED staff, and my heart broke for them. I also heard that the hospital had three other coworkers who had passed away from COVID-19 as well. COVID-19 does not discriminate! I took care of a 94-year-old man whom I discharged home who was tolerating the virus just fine, and the next minute, we were intubating a healthy 37-year-old.
One night on my way back to the shuttle, I saw the staff taking a patient who passed away out to the cooling trucks parked on the side of the hospital. This was very emotional for me. I can’t imagine how hard it was for patients' families not to be able to be with their loved ones while they passed, and then to have their bodies put in a truck to wait until they can put them to rest. I'm not saying that putting bodies in these trucks was cruel or unjust; NYC is just doing what they can during this unpredicted and overwhelming time. I saw my share of sad things happen, but I want to say that the number of positive things I saw, outweighed the negative by far. NYC has the most amazing people, and I'm saying this of every person I met, whether working with them in the ED or just in passing. I have to say that NYC has not let this defeat them! They stood up and fought and are winning! There were only around 300 deaths in the past 24 hours in NYC the day I left, and the ICU I worked in was empty!
I'm so grateful for this opportunity.
Thursday, May 14
Reflections from the frontline: ‘He kept calling me "his personal angel" every time I came into the room.’
Rylee Utley, RN, Life Flight nurse based out of Dixie Regional Medical Center, shares her perspective after being one of 100 caregivers deployed to New York City as part of Intermountain’s COVID-19 Response Team. Rylee was at NewYork-Presbyterian’s Southside Hospital in Bayshore, New York.
When I received the email about the opportunity to go help in New York, I had an impression that I needed to go. I wanted to help our fellow nurses and healthcare workers who were experiencing such a large surge and chaos. I didn't really even debate whether or not I should go—I knew I needed to. I feel so honored that I was chosen to go; so many other caregivers would have gone if they had the opportunity. That's what I love about Intermountain and our staff. We have this culture to make a difference that is just engrained in us.
Nurses Rylee Utley (left) and Libbey Steed outside Southside Hospital’s emergency room during their night shift.
My background is primarily in the emergency room and I was recently hired on with Life Flight's fixed wing team as well. While in New York, I was in the ER for 10 out of my 12 shifts, and also jumped on 2 ICU shifts. There are so many personal stories I could share about interactions with patients and staff. One story that really stuck with me involved a gentleman I took care of in the ER. It had been a busy day and he was feeling scared and alone. I was able to move him from a hallway bed into a shared room that had a curtain divider, get him adjusted and more comfortable, and then educate him on what was going on with his care. I was able to update his family for him. (His phone was dead and he had not had contact with his family all day.) I felt lucky to make a little difference for him and his family as I provide the update. He kept calling me "his personal angel" every time I came into the room. He also sang a song to me on a few occasions when I went into his room. I can't remember the name of it, but it talked about standing with your friend and lifting them up in a time of need. And remember—I didn't do anything extravagant for this patient—I just gave him some of my time and tried to bring him a little bit of peace in scary moments of uncertainty so that he didn't feel alone. That's what being a nurse is to me: making a difference for your patients. It doesn't have to be an extraordinary measure; just taking the time to hold a hand, and be a friendly face to someone can make a huge difference.
Another thing that made me so proud when we were in New York was that we were known as "The Utah Nurses." After a few days, we stood out to the staff we were working alongside. They knew the Intermountain nurses and loved us, and we loved working alongside them and helping (even though it was very tiring). The culture and work ethic we have at Intermountain Healthcare is phenomenal and people notice it. We have a culture that I feel is effectively explained in our healing commitments:
- I help you feel safe, welcome and at ease.
- I listen to you with sensitivity and respond to your needs.
- I treat you with respect and compassion.
- I keep you informed and involved.
- I ensure our team works with you.
- I take responsibility to help solve problems.
People felt that culture from us, and I was so honored to represent Intermountain while in New York. The healthcare workers there remain in my prayers every day—hoping they’re able to recover soon. They’re amazing. The hardship they’ve endured seems insurmountable, yet they’re still showing up every day and pushing through and fighting. They’re inspiring and are the real heroes.
Rylee and other members of Intermountain’s team deployed to Northwell and NewYork-Presbyterian join for the nightly “7:00 Cheer” conducted by the New York Fire Department.
Wednesday, May 13
Reflections from the frontline: ‘This virus is mean.’
Kimberly Di Ciolli, RN, Intermountain Medical Center, shares her perspective after being one of 100 caregivers deployed to New York City as part of Intermountain’s COVID-19 Response Team, at NewYork-Presbyterian’s Columbia Medical Center.
When I saw the email from HR sending an open invitation to join the Crisis Relief Team (now known as the COVID-19 Response Team), I felt it was an answered prayer to serve. I was very grateful when I found out I was chosen to go. Two days later I met with the team and we were on our way. I was deployed to Columbia Medical Center, one of the New York-Presbyterian hospitals. I was impressed and humbled hearing how fast and responsive they were system-wide in creating more hospital beds (converted the OR, cath labs and med/surg units to ICU), and how their Children's Hospital was accepting patients up to age 40. I was stationed in the Emergency Department at Columbia. My first day was an eerily quiet start; even the nurses I worked with were surprised. They would share stories about how busy their ED had been, up to 250 patients at one time. They shared their experiences from weeks prior about how they placed the beds closer together to have more patients near oxygen flowmeters, while many others were still waiting in the hallways. They shared how oxygen tanks had to be checked and changed every 90 minutes and how helpful it was to have a person's sole focus be to check and change them. There was a lot of sadness as they talked about how one of their nurses that was intubated, and sadly passed away my second week there.
Challenges with intubation
Before I left Utah, I started seeing acute respiratory distress syndrome (ARDS) in COVID-19 patients and was thinking I was prepared for that. When I got to New York, I learned how they would try to hold off intubation as long as possible in the Emergency Department, or do a more controlled intubation with the anesthesia team. Working with their ethics team, the physicians also would start having these difficult conversations early with family members regarding palliative care options and conduct do not resuscitate/do not intubate (DNR/DNI) conversations through FaceTime. This was due to the grim mortality rates they were seeing with the patients they intubated prior for ARDS.
Connecting patients with interpreters and family
There was an older woman who was struggling to breathe and was very anxious. We put her in an isolation room on a bipap machine to try to turn it around. She wasn't getting any better. She spoke Spanish and wanted us to call her daughter. In my mediocre Spanish I was able to spend some time with her and communicate a bit while we waited for an interpreter to become available and connect her with her family. She seemed to calm down a little so I stayed as long as I could. They were able to get a Spanish interpreter to help us answer all her questions. We were able to contact her family so that they could be there. I had to hand over her care before I saw the outcome, unfortunately. The ED had an ICU holding area, and I didn't see her there after that day.
“He was in his 30s, healthy and resilient.”
My last day was in an area meant for patients with urgent needs, but would typically be discharged home. I had a patient that had been fighting the COVID-19 infection for nine days. He was in his 30s, healthy and resilient. He had been seen twice for the same infection. He went to the ER four days prior and was sent home with a home pulse ox to monitor his oxygen saturation. He returned because his oxygen levels dropped to 87%. He was placed on increased oxygen to try to delay possible intubation. We tried to bring his oxygen down to 4 liters/minute, but he didn’t tolerate it well and was placed back on a higher oxygen setting. He was sitting up, not comfortable, but he was calm. Every time I went in the room we would joke around. I don't remember specifics anymore, but I remember his eyes. He was able to connect with his family on his phone. He was still able to laugh and have hope in his eyes. He was to be admitted to the step-down unit. I wish I knew his outcome. I am still rooting for him.
“Patients were so very sick, but it didn't take their spirit.”
In those two weeks in New York, I saw so much fear in patients’ eyes and voices. Many patients were anxious and were afraid to be alone. Other patients were very tired, families cried on the phone saying goodbyes. These families heard so many hard messages over the phone. Patients were so very sick, but it didn't take their spirit. They smiled, they laughed, they joked. This virus is mean. Through diagnostic tests I saw how it occupies a lot of space all over the lungs, decreasing air volume, makes their blood very hypercoagulable leading to blood clots all over the body. It put strain on the heart both physically and emotionally. It puts patients more at risk for heart attacks, stroke, pulmonary embolism, ischemic injury to a limb because of the blood clots. So many were put on blood thinners in the Emergency Room.
“We can protect a lot more people”
Fortunately, the number of new active cases were declining when we arrived because people were staying home, slowing the spread. The ED was not overwhelmed anymore as the city was also shut down. Many nurses, techs, housekeeping staff kept expressing their fear of a second wave as things open up. At home, Utah Leads Together 2.0 is Governor Herbert's comprehensive task force plan that is giving guidelines to follow and continually evaluate to safely move forward. While it may not prevent the illness, we can protect a lot more people if we implement and follow guidelines to help slow the spread.
Tuesday, May 12
Reflections from the frontline: ‘I put my head down and went to work because I felt I could handle it all.’
Elizabeth ‘Liz’ Hyde, RN, BSN, Intermountain Medical Center, shares her perspective after being one of 100 caregivers deployed to New York City as part of Intermountain’s COVID-19 Response Team, at Northwell Southside Hospital in Bayshore, New York.
New York will always hold a special place in my heart. After coming off of my own personal trial, I felt like going to New York would enable me to step out of my own life and go help those who needed help and were living a harsh reality — harder than what I was personally dealing with.
Walking into every shift in New York, you never knew what you were going to experience. When I look back through my experiences, one shift in particular comes to mind. I was given the assignment of three intubated, very sick patients. I felt like I was jumping from one patient to another dealing, with different issues. I was lucky enough to have a patient assignment next to Chad Nielson, another nurse from Intermountain. Chad was given a less difficult assignment and was constantly offering to help me. Being an ICU nurse, I put my head down and went to work because I felt I could handle it all.
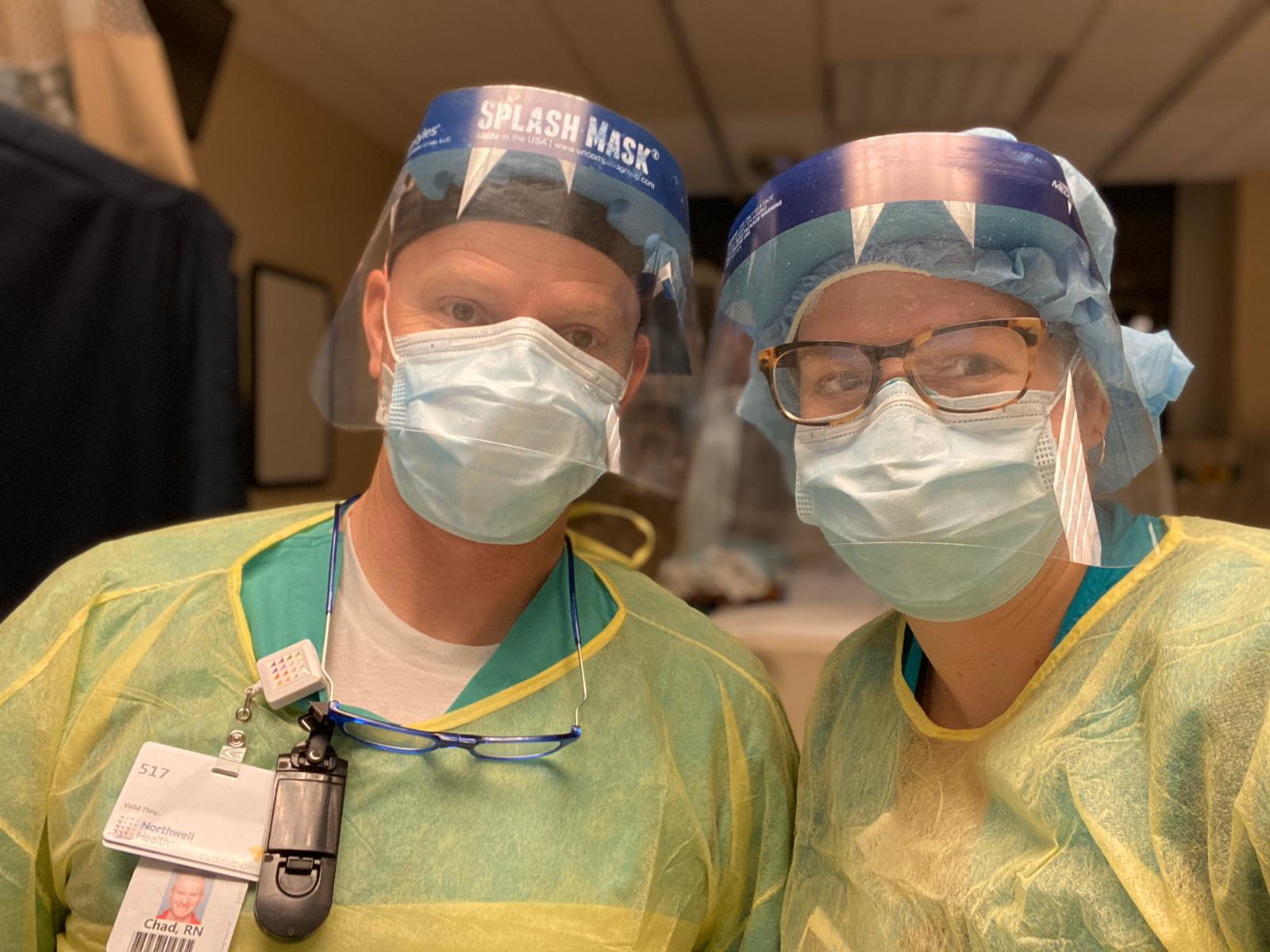
Liz Hyde, RN, and Chad Nielson, RN, both based at Southside Hospital
One of my patients was very anxious. She had been intubated, extubated, and then re-intubated. She was constantly tapping to get someone’s attention. Without family at the bedside to comfort her, she wanted anyone there to hold her hand. I went to comfort her as much as I could, but I was busy, running to and from, here and there. I told Chad about her and her story. The next time I walked past her room, there was Chad, sitting by her bed holding her hand. I was caught off guard. I went and did what I needed to do with my next patient, and came back into this patient’s room. Chad was still there, holding her hand. Over the next three nights, Chad and I were assigned patients next to each other and each night Chad would take time, two to three times a night, to go hold this patient’s hand.
I'm grateful for the opportunity I had to go to New York — not only because I was able to help people in New York, but I met some amazing people I work with here in Utah. The relationships I was able to make with some of these amazing nurses I will never forget and am so grateful for them.
Intermountain nurses Liz Hyde and Michelle Bryce with the Northwell Southside Hospital MICU/SICU teams
Monday, May 11
Reflections from the frontline: ‘He asked the doctor and I to tell his wife how much he loved her.’
Sam Murray, RN, Primary Children’s Hospital, shares his perspective after being one of 100 caregivers deployed to New York City as part of Intermountain’s COVID-19 Response Team, at NewYork-Presbyterian’s Columbia Hospital.
I wanted to take a moment to share a few of my experiences while working with the Intermountain COVID-19 Response Team at New York-Presbyterian Columbia. I’m so thankful for the experience I had and that I was granted the opportunity to go. It was incredible, while also being one of the most challenging and heart-wrenching experiences of my life.
During my time at NYP, I spent most of my time working in a shared step-down ICU and ICU combined. I also spent a few days with the Prone Team. Prone positioning is when you assist (move) a patient from lying on their back onto their abdomen. To put it short, being prone helps the lungs expand in order to ventilate more effectively. Proning a patient sounds simple, but the process can be quite complicated. The patient being proned is intubated and on ventilators, has several IV lines and drains, and is sedated and paralyzed. The prone team consists of six members. One of the members is a nurse and their role is to keep track of all the drips and ventilator settings. They also make sure that patients are on certain medications at the correct dosage. Another member of the team is either a respiratory therapist or a physician to secure the endotracheal tube. The rest of the team consists of occupational and physical therapists to physically perform the turn. These professionals have become really good at this procedure, which can be frightening at times. One day we went to prone a patient on our list and a physician informed us that they were beginning the process of withdrawing care. Come to find out, this patient worked as a nurse in the Emergency Room at NYP. That was really heavy for me. Before I came to New York, I knew healthcare providers were contracting this virus and some even having their lives taken by it, but it was devastating to see firsthand. Not to mention, the nurse manager for the unit that I was assigned to was hospitalized during my time at NYP. I never had the opportunity to meet her.
The hospital had previously shuffled units around in order to increase their ICU beds. (This is very common in New York City during the pandemic.) The OR converted most of their rooms into an ICU. There were three patients in each of these OR rooms. They made their cardiac catheterization lab and an auditorium into ICUs as well. The way New York-Presbyterian adapted was amazing.
On one of my first shifts, I had a patient who was on a lot of oxygen and the doctors were trying to do anything to prevent intubation. The reason they do this is because many patients stay on ventilators for a long period of time without improvement. He was on two different types of oxygen in an attempt to support him. He was on maximum settings of High Flow Nasal Cannula, plus nonrebreather at the maximum flow. The patient progressively declined. His oxygen saturation was consistently in the 70s, his respiratory rate was high, and he was working really hard to breath. I notified the physician resident and we waited a little while to see if the patient would improve, but unfortunately, he didn’t. The doctor explained to the patient that he required intubation. This patient’s wife was also hospitalized; she happened to be one of my patients as well. He asked the doctor and I to tell his wife how much he loved her.
On my last day, there was a patient getting transferred out of the ICU to a lower acuity floor. A group of us lined up in the hallway and we clapped and cheered for her as she went by on a stretcher. She had a mask on, but I could tell that she was smiling. She also had tears rolling down her face — and so did I.
It’s difficult for me to put into words how much this experience has impacted me. I’ll never forget the strength and resilience of those in New York City and I have the utmost respect and praise for them. I have no doubt that they will come out of this stronger. I’m going to hold my loved ones extra tight.
Members of NewYork-Presbyterian’s ICU team
Friday, May 8
Reflections from the frontline: ‘To set the record straight, the stories are real’
Rachel Gathro, a RN at Intermountain Medical Center, shares her perspective after being one of 100 caregivers deployed to New York City as part of Intermountain’s COVID-19 Response Team, at a Northwell Health hospital.
I went for many of the same reasons everyone else in our group went. I went to help and I went to learn. When I heard Intermountain was putting a response team together, I felt like I needed to go. This is why I became a nurse. I don't like the term "hero." This is my job—to help others when they can't help themselves. However, when I found out I had been chosen to go, I suddenly got a little nervous. I had heard the same stories all of you have about how COVID-19 has impacted New York and I wasn't sure what was real or what I was going to encounter there. And to set the record straight, the stories are real.
My RN background is emergency medicine, so I was assigned primarily to the ER with a couple shifts in an ICU. The nurses in the ED said that they were at work one day and everything was normal, and they came back the next day and suddenly their ED was overwhelmed with people dying of COVID. They said it was literally from one day to the next. Patients were mostly in curtained rooms, 2 patients to a room, and patients were in the hallway. I arrived days after the numbers of patients started decreasing and this is still what I found. Resources were limited and nurses were emotionally and physically exhausted. In New York, at baseline, patients sometimes have to stay in the ED for a long time waiting for a room upstairs. During this pandemic, it was even more common. I was told that prior to my arrival they were holding about 70 admitted patients in the ED at a time. They have created new units in tents and meeting rooms to make space for the increase in patients, but there are still so many.
Families weren't allowed to come in to stay with the patients unless they were actively dying, so when I had time, I tried to provide what comfort I could to my patients. I had a patient who was put on palliative care because of complications from COVID. She spoke two languages, but neither was English. Fortunately, I knew some of one of the languages she spoke. I tried to make her physically comfortable and reassure her I was here for her if she needed it. She was able to get a room upstairs the next day. I had another patient who had a panic attack because of the stress the virus was having on her day-to-day life. After I made sure all my other patients were stable, I talked with her for a while, answering what questions I could about the virus, what she needed to do to stay safe, and reassure her of the hope that she could have. She was able to go home. In the ICU, most patients are intubated. I had one patient who wasn't, but was very confused. She had a bleeding disorder combined with the bleeding issues COVID causes. I had to hold pressure on a wound for 45 minutes without moving my hand to get the bleeding to slow down. As I held pressure I tried to talk to her so she wouldn't feel alone. She passed away the next morning after going into cardiac arrest.
With so many unknowns and poor patient outcomes, moments like these helped strengthen me as I tried to make a small difference in New York.
Reflections from the frontline: ‘This virus does not discriminate.’
Michelle Hicks, RN at Primary Children’s Hospital, shares her perspective after being one of 100 caregivers deployed to New York City as part of Intermountain’s COVID-19 Response Team. Michelle worked at the NewYork-Presbyterian Columbia Hospital in many departments.
I arrived in New York, two days after receiving notification about a deployment to help my fellow nurses in NYC. All I knew was I was going to be working at NY-Presbyterian’s Columbia Hospital—also known as the Milstein building. The next day was orientation where the administrative team welcomed us and took the time to prepare us for what we were getting ready to walk into. This was ground zero.
My first three shifts in the ED (emergency department) were not that bad, but this team had been in hell for 6 straight weeks before we arrived. They actually all agreed we were the “white cloud” – a bright spot after a storm. They needed us to hear their stories though, they needed a shoulder to lean on. Most of the staff were staying in dorms to keep their families safe. One male nurses had not seen his newborn son in 5 weeks. This virus was killing their own, too. I heard them say multiple times, “This virus does not discriminate.” This same team lost 32 patients in one day. I silently prayed for them, while I watched them work as a fluid, well-oiled machine.
Shift 4 out of 9 got real for me. I was asked to work in the makeshift OR intensive care unit. The Columbia Hospital usually has about 120 ICU beds; post COVID-19 surge, they have about 260. I had three patients and I called them all by their first name. They all had been on breathing machines for over a month as well as multiple drips that I had to adjust hourly to keep them alive. They were alone; no family due to visitor restrictions, just fighting for their lives—the strongest of strongest fighters, I think. I had a staff nurse who walked around with me to see her fellow coworkers who were now ICU patients. She didn’t want to walk by their rooms alone… All she wanted to do was to see if they were alive. She also wanted me to hear her stories. She survived COVID-19 and this was her first day back to work.
Another ICU shift I took care of one of their own doctors. For two days, we fought to keep this man off a breathing machine, but on day 10 of illness, he agreed it was time; he was tired. He knew we did the best we could. The last words he said to me were “God bless you” before we took over breathing for him.
Yes, this virus is attacking the weak and vulnerable humans of the world. But does that mean just because you’re over 35, you’ve made bad health choices in your life, or have inherited family genes that you do not deserve a chance of being protected? This is not about your inward views on life, it’s about protecting humanity as a whole. It’s about a struggling healthcare system that needs to pull together to save humans. Look at others, not yourself.
This was why I became a nurse, these moments right here: to cry with my patients, to mourn a loss, to fight for the weak, to work side by side with some of the strongest leaders, to watch in awe a team work together in disaster mode, and to dance and sing at the end of it all! I have always wanted to be a frontline worker and will always be one. Please do not forget the NY nurses—this is not over. Pray hard for them. I will forever be grateful they welcomed me into their home for two short weeks with open arms.
Intermountian caregivers at orientation in New York.
Thursday, May 7
Reflections from the frontline: ‘All I could do in that moment was cry and tell her ‘you’re welcome.’
Tiffany Miller, a RN at Alta View Hospital in the emergency department, shares her perspective after being one of 100 caregivers deployed to New York City as part of Intermountain’s COVID-19 Response Team. Tiffany was based at the New York-Presbyterian Brooklyn Methodist Hospital.
When I was five years old, I had a traumatic event occur involving travel and the unexpected death of my grandfather. This event left me with several unanswered questions. This event led me to pursing an interest in healthcare to find my answers and to provide those answers and comfort to individuals in similar situations. I was also always intrigued when my mother would tell my family stories that my grandfather told her when he served as a medic in WWII.
Since this event, I never traveled alone as an adult and when I have traveled in the past, it has been anxiety provoking for me. When I received the broadcast email asking for volunteers to go to New York I immediately responded. Ever since I heard in the news that New York was an epicenter of COVID and so many people were suffering, I felt this constant obligation to help my fellow nurses and healthcare workers. I did not feel the anxiety that I normally do right before leaving out of town. I am not much of a spiritual or religious individual but I don’t think I have ever prayed so much to have my grandfather be with me and protect me from this illness while serving in New York.
It was a decision that my family did not take lightly. Family, friends, and co-workers were questioning my decision to go and why I would leave my two small children behind. Others asked why I’d leave during finals for the FNP (family nurse practitioner) program I am currently enrolled in. I simply responded to every question asked that I don’t know why, but I feel like I needed to go and help. I could not provide them with a better answer. The administrative staff were all so kind, welcoming, and flexible. I was initially assigned to the Emergency Department at the Brooklyn Methodist Hospital for New York-Presbyterian. I asked to work in the ICU instead since I already have quite a bit of experience in Emergency Medicine back home.
During my second shift, I provided care to an intubated COVID positive male in his 30s. He had been intubated for over three weeks. The nurses were so busy with their 3:1 (patients to caregiver) assignments that they did not have time to provide basic cares such as turning these patients every two hours (a common, unfortunate consequence of crisis level care). Since he was my only assigned patient during this shift, I made it a priority to communicate and coordinate a time with ancillary staff to give this patient a bed bath and include oral care which the patient really needed. We had just finished giving this patient a bed bath when his brother called and asked to FaceTime with his brother. The patient’s brother repeatedly commented how well the patient appeared and was thankful to the CCU staff for taking great care of him. Simple comments like this just reaffirm that nursing was the correct career path for me.
I was the primary nurse to another intubated COVID positive patient in his 60s during several of my shifts. I got to know his daughter very well. During my last shift, she called for an update and I provided her a basic, but encouraging update. She then thanked me for coming out to New York and told me a few times that she thought I was a great nurse and was so appreciative of the care I provided to her father. All I could do in that moment was cry and tell her “you’re welcome.”
I am so grateful that I was selected for this eye-opening and educational opportunity. Thank you again to Intermountain and to the staff at the Brooklyn Methodist Hospital for arranging this opportunity. I will never forget it!
Saturday, May 2
From the frontlines – Day 17, NewYork—Presbyterian
Message of praise from Dr. Harland Hayes, speaking to his fellow caregivers deployed to support NewYork—Presbyterian hospitals.
Job well done, everyone! You’ve made an impact that has caught the eye of the nation. You’ve endeared yourselves to our new friends at NewYork—Presbyterian. The support they’ve felt from you has meant the world to them as their backs were breaking under a load too heavy to carry. You will never look at New York City the same way; the next time you come, the horns will be honking, the streets will be full of people, talking and laughing, and in your quiet moments you’ll remember the privilege it was to play the role you did in the Big Apple during this pandemic. This city will forever have new meaning for you that words can’t express. But, as always, and most importantly, at the heart of this trip and of your time here was the individual patient. You took your empathy and your skills across the country and touched individual lives – thousands of them. They may not have known you were from Intermountain, and their families weren’t there to thank you and to ask for your story, but their families and millions across the country have been hoping and praying that they would be helped. And you responded to that call. I can’t imagine better care, I can’t imagine a better crew!
A warm welcome at Intermountain’s Employee Services Center, where returning caregivers received post-deployment testing for a quick transition home.
Reflections on the deployment to the New York Presbyterian hospital system from Brad Whitcomb, RN, from Utah Valley Hospital
Almost two weeks ago I came out to NYC to help and be of service to both the people in the New York that were ill and my fellow healthcare providers. With almost 99 other coworkers from Intermountain Healthcare, we came out here not knowing which hospital or department we would be working in. There were many unknowns for us, but what we did know is that we all felt this urge, this pull to come. We knew that if we were able to go, we should. I found out about this opportunity to travel to NYC exactly one week before I left.
I was humbled, or at least I thought I was, then I got to the hospital. We met their HR team and other administrators, who gave us a tour of the hospital. They went over cold hard facts and numbers with us. They did this not to scare us, but to prepare us. They showed us the ER, OR, and the PACU that were converted into an ICU (punch out this wall or make a hole in this wall, now make a tent like wall, they had to create negative pressure rooms where there weren't any before), the same goes for the ICU. They had to quickly make their ICU that only had five negative pressure rooms into all negative pressure rooms. When we got to the ICU it was good that I was wearing a mask because my jaw was slack with shock. A few of us must have still looked like deer in the head lights (or maybe just me), because I remember our tour guides asking us several times if we were okay. Every room had an isolation supply cart outside of it. Every patient that i saw was on a ventilator. Almost every room had two beds in it with enough room for a RN or RT to get access to the head of each bed. Because of the severity of the disease, many patients were on dialysis or something like it called CRRT. I thought to myself, “I don't know if our hospital systems are prepared for this.” Then I thought it’s a dang good thing that they sent us out here. It’s good that they sent doctors, PAs, NPs, and administrators. People in the right positions to get us prepared for what could happen in Utah.
Then I saw a nurse come out of a patient’s room. She washed her hands, grabbed some meds from the med cabinet, then sat down and put her head in her hands at her desk. She took a quick breather, got back up and started to get back into her full PPE to go back into the room to give the medications to the patient. I thought, “This is why I’m here; this is why they sent RNs.” We’re here to care for, to learn from, but also to give relief to those that provide care. I have seen patients die and patients get better. I’ve learned a lot. I’ve seen some amazing leadership. I’ve met some of the strongest and most awesome caregivers. While in the face of all that is happening around them, they can still laugh, they can still find happy moments, they can still find the best during the worst. They are extraordinary people! Their teamwork is above and beyond, they anticipate each other's needs. I have now seen angels at work. I am humbled. These are the true heroes!!
Friday, May 1
From the frontlines – Day 17, Northwell Health
“You have been absolutely terrific. Thank you,” said Northwell President and CEO Michael Dowling as he addressed Intermountain's team before they left New York. “We were hit by a tsunami, having seen about 39,000 COVID-19 patients overall. When we reached out, Intermountain could not have been more helpful and moved very quickly. The assistance you provided was extraordinary.”
The trip home, with water cannon tributes from appreciative airport workers in both NYC and Salt Lake City.
Homecoming tributes for our brave coworkers.
A last word from the frontlines – What the name “Hero” means to me
This post was authored by Libbey Steed, an RN at Dixie Regional Medical Center, about her thoughts and feelings surrounding her experience in New York as part of Intermountain’s COVID-19 Response Team.
When I submitted my application to come to New York City during the current pandemic, many people questioned my decision. They asked me about my reasoning and wondered why I would willingly place myself at risk for exposure to the deadly COVID-19 virus. I could not explain to them why I felt compelled to travel 2,200 miles across the country and help people in the middle of this crisis, but I know why I made that choice. When we arrived, our team was referred to as “heroes” and I could never understand why. We were simply doing a job that others had been doing diligently for months. There have been happy times, hard times and very humbling times.
However, today’s date is nostalgic for me and truly helps me know WHY I’m in NYC. On 4/26/2017, I was in an ICU hospital bed at Intermountain Medical Center in Murray, Utah. I was intubated and taken to emergency surgery to have a colectomy that many thought I would not survive. Throughout my own personal crisis, my hospital staff provided hope, comfort, love and support. My medical team MADE me survive when the odds were grim. My medical team became my “heroes.”
Three years later, I’m standing at the doors of Southside Hospital in Long Island, New York in the middle of the New York City COVID-19 crisis working as an emergency room nurse because this is what I was made for. Today, I know without a doubt why I survived. I survived to provide hope, love and comfort to those in need during this crisis.
Every day here has been a hard day but filled with many little wins. Maybe we helped someone breathe that could not, maybe we held their hand and provided comfort, maybe we offered a smiling face. Every day we do something for patients that has helped make life during this difficult time a little better, hopefully a little easier.
As healthcare professionals we feel compelled to be a smiling face when inside we really want to cry, to be stoic when the odds of survival are not great for so many. Even during a pandemic, we continue to believe that our next patient is “the one”—the one that will recover and live to be a “hero” for the next person.
Today, I am humbled to be considered a “hero” for someone else and I am grateful for the opportunity to serve in New York City!
Libby Steed, RN, after she took of her n95 mask following a 12-hour shift.
From the frontlines – Day 16, NewYork–Presbyterian
Parting words of praise to the caregiver team deployed to the NewYork-Presbyterian hospitals by Aaron C. Wood, CEO/Administrator, Sanpete Valley Hospital.
"Ok, gang, the end is just about here. I hope you will each look back on this experience with the proper amounts of sadness, reverence, pride and sheer joy at this incredible opportunity. I can't wait to hear, share, and trade your stories.
For several days now, I've been regaled from every direction of NYP leadership of how magnificently you have each performed. The gratitude of our hosts is as poignant as it is sincere. I add to the NYP chorus: thank you. Great job. Well done.
I have never been more proud to be associated with you and all that Intermountain Healthcare is, than right now. As we like to say in Sanpete...You don't suck.
See you back at the 'Crossroads of the West!'"
Thursday, April 30
From the frontlines – Day 16, Northwell Health
Intermountain’s COVID-19 Response Team from Northwell Health team is returning home today. This post was authored by Dr. Jarid Gray, a hospitalist at Cedar City Hospital, about his thoughts and feelings returning home.
Our time with the COVID response team is coming to an end. We are hopping on the plane back to Utah. I have a few take home messages that I want to share.
To the people of New York:
You have taken the brunt of the storm. In doing so, you have had to deal with grief, fear, and sorrow in ways that most people cannot understand and will probably not have to experience. Your mettle has been tested, and you have been found to be up to the challenge. It warms my soul to watch your resilience in the face of disaster. The strength of the human spirit is a beautiful thing, and you have exhibited it for all of us to see. The welcome that you offered our team will not be soon forgotten.
To the people of Utah:
I know many are skeptical of the impact of this Coronavirus because there hasn’t been the case load or deaths in our state. I will tell you with utmost sincerity, we do not want to see this disease darken the doors of our homes and hospitals. In my 20 years of being a physician, I have never seen a disease utterly dominate an entire hospital. This disease is unprecedented in the volume of cases, and the severity of illness. I have responded to more rapid response calls (patient in distress) in the last 2 weeks than I have over the course of my entire career. I have heard more code blue calls in one day than I have heard at our hospital over the course of a year.
Be patient with the restrictions. Be vigilant at protecting those who are at highest risk. Be prepared with adequate supplies at home if we were to see this severe of an outbreak in our state.
To the physicians, nurses, staff, and administration of Northwell Health:
I thank you from the bottom of my heart for the welcome that you have offered us. I appreciate the patience that you had as we learned the computer system and the workflow. I marvel at the grace and fortitude shown by your caregivers as they battled against an indomitable disease. When I realize the fact that you have been working with this absolute tidal wave of sick patients for over 6 weeks, it raises my admiration for you all even more. I am grateful that you have been willing teachers. I wish you the best of luck as hopefully your lives return to closer to normal over the next few weeks.
To my fellow teammates here in New York:
Wow, what an unforgettable experience. Whenever I hear “Here Comes the Sun” in the future, I will be immediately brought back to April 2020 when a brave group volunteered to go into the belly of the beast to assist in the war against COVID-19. I will forever be grateful for the discussions on the rides to and from the hospital, and the debriefing/decompression that happened during our trip.
To my fellow caregivers in Utah:
First of all, we got this. I know your character, your professionalism, and compassion. We have what it takes to manage and persevere if we were to see this magnitude of outbreak in our state. I think we have prepared about as much as we can. We won’t know what will work, what won’t, until we are in the crucible. I am excited to discuss what I have seen and learned here with everyone when I get home.
To my family:
I could not have done this without your support. I could feel your love and prayers every time I woke up, every time I entered the hospital, and every night that I went to bed. I know you worried for my safety. Be calm, knowing that I took all precautions and wore all my protective gear to reduce my risk as much as possible. I love you all and cannot wait to see you again.
This post was authored by Katie Cutting, an RN at Intermountain Medical Center, following her 2,200 mile journey to help caregivers in New York City. These thoughts were written after one of her final night shifts at Northwell Health’s Southside Hospital.
I’m a Medical-Surgical (Med-Surg) nurse. The COVID pandemic has created a large number of very sick, ICU level patients. Here in New York, Med-Surg nurses have been floating to ICUs to work as “functional nurses” assisting with the care of ICU patients. The ICU nurses have been facing ratios of 1 nurse for 4 critical patients, or even up to 1 nurse for 5 critical patients. With these ratios, having additional support is absolutely necessary. Due to limited staff numbers in light of the pandemic, this meant that a few weeks ago only 3-4 nurses would be left to cover a 40+ bed Med-Surg unit, while the rest of their team worked in the ICU.
Our Intermountain Healthcare team is primarily made up of ICU and ER nurses, so it felt really special to also support the Medical-Surgical units at Southside Hospital. These nurses have gone through so much. Their stories are beyond anything I could imagine. They have been responsible for up to 10 moderately acute patients at once. (For reference, on my floor at Intermountain Medical Center, our upper limit is 6.) Not to mention, these patients can go downhill fast. One nurse shared a story of having three “Rapid Response” calls on the floor in one day, all at the same time, and all three patients needed to be intubated and transferred to the ICU. Maternity was turned into a COVID unit one day when they needed more beds. A nurse recalls walking into the supply room there, spinning in a circle looking for oxygen supplies, and finding only diapers. They ran out of actual hospital beds. Instead, every patient was on a stretcher, needing to be manually lifted up and down to “raise the head of the bed.”
When we arrived for our first shift at Southside Hospital, a tent was opened for patient care 3 hours prior. The tent (also called the Annex) was an open unit of all COVID-19 positive patients who met certain criteria of stability. This tent is where I spent my first night at Southside Hospital. That night was quite a learning experience for everyone. The heater was so loud you could barely talk, yet despite the blasting noise it was still very chilly. We spent the shift making a list of supplies that we needed for patient care. The patients were in open stall-like rooms, with a portable divider that we could put in front of their bed for privacy. I could sit at the “nurse’s station” (a table with laptops) and look around, seeing all of my patients in one glance. The overhead lights did not dim until 23:00 (11 p.m.), and even then it was still bright enough that almost every patient had an eye mask on. I was assigned to the tent again for my second night, and it was significantly improved. The noise was manageable, temperature controlled, supplies available, and we were able to dim the lights earlier in the evening. The response to our concerns and requests was answered quickly and efficiently.
Week two I worked on my “assigned floor,” which was 6 Tower. From what I understand, this inpatient unit typically functions as a mix between caring for long-term tracheostomies, video EEG monitoring, and patients from psychiatric facilities requiring hospitalization for medical concerns. Now of course, the whole unit is COVID. Walking into the unit I make sure my N95 is in place. While patients are in rooms with doors and there shouldn’t be any aerosol generating procedures going on, you can never be too careful. At the maximum I had 7 patients on a night shift, mostly averaging around 5 patients a night. Things are getting more manageable. There is some sense of a gradual return to normal. A collective deep breath being let out.
My final two shifts I got to experience another kind of unit. “Transitions” is a clean (read: non-COVID) unit, caring for standard Medical-Surgical patients who received a negative COVID-19 swab. The room was originally the “Theodore Jospe Board Room,” turned into a 15-bed open unit. Curtains were installed, a call light system, and electrical outlets at each bed space. Two tall shelving systems contain the unit’s supplies. Tables in the center of the room make the nurses station. The kitchenettes and sinks were already available, although a medication fridge has been added, as well as a Pyxis medication delivery system. The cafeteria hallways bathrooms have become patient restrooms.
It's incredible to see what has been done to accommodate care for the overwhelming influx of patients to the hospital. When the ICUs were full, some Medical-Surgical units were converted to ICUs. When more Medical-Surgical rooms were needed, new options were developed. The resilience, ingenuity, and resourcefulness of these health care workers, administrators, and team members is incredible to witness to. They've been living through one of the most traumatizing experiences I could imagine, and they're still finding ways to be positive, connect with one another, and laugh together. It's been the biggest honor and privilege of my nursing career to come to New York and work with and learn from these real-life healthcare heroes.
Katie is one of 11 Intermountain caregivers assigned to the Southside Hospital overnight shifts.
From the frontlines – Day 15, NewYork–Presbyterian
Here are a few photos taken by the Intermountain team of caregivers deployed to NewYork-Presbyterian hospitals.
Wednesday, April 29
From the frontlines – Day 15, Northwell Health
Rachelle Rhodes, RN, Intermountain’s executive director of emergency department and trauma operations, Paul Sharp, nurse practitioner at Salt Lake Clinic, and Adam Phillips, physician assistant at Utah Valley Hospital, discuss what New York’s hospitals have done to heroically respond to the pandemic by quickly making ICU capacity to treat critically ill patients, and the important lessons learned for Intermountain.
This post was authored by Adam Phillips, physician assistant at Utah Valley Hospital, following his 2,200 mile journey to help caregivers in New York City. Adam is one of 50 caregivers deployed to help at Northwell Health and is at Long Island Jewish Medical Center.
As both a human and clinician, what New York has been enduring for nearly two months has been fascinating to me. Call me a weirdo, but for the past three weeks or so, I've done my best catch New York Governor Cuomo's daily press conference. I couldn't fathom the tidal wave of COVID patients that had swallowed their city and state.
On April 8th, a friend and colleague shared a video with me, sent to him by his brother who had volunteered to help in NYC. The video was of one of the hospital wards he had been assigned to. The circumstances shown in the video left me speechless. I couldn't believe that such circumstances could exist in the developed world.
As a result of the video, I felt compelled to help. This happened to correspond with Intermountain's request for volunteers to be deployed to assist in NYC. I put my name in the hat and was selected to participate. With just a few days’ notice, I got ready. I'm so grateful to my team members on the Utah Valley Trauma Team that stepped up and absorbed my clinical responsibilities for basically three full weeks within 5 minutes of a text message letting them know I was going. My wife and daughters have also been continuously supportive.
After a half day of orientation, we jumped in. With my clinical background and at my request, I was placed in a rotation covering in their critical care units. As a result of COVID, Northwell Long Island Jewish Hospital has had to more than triple their critical care beds, covering 9 distinct units, constituting hundreds of beds. These units were thrown together is such places as their post anesthesia care unit (PACU), med surgery units, post cath recovery unit, among other places.
The sheer volume of the high acuity is overwhelming, and I've only had a two week of tasting this. Every unit is filled with critically ill, intubated patients. Most are on vasopressors; many are on multiple vasopressors. 25-30% of the patients require dialysis, generally continuously. In the patient population that deteriorates to require an ICU setting, nearly every organ system is being injured. Strokes, intracranial hemorrhage, liver failure, bowel perforations, limb threatening ischemia, among other problems are all happening as a result of COVID infections, in addition to the well described lung and kidney issues. The underlying patho-physiology of all of these changes is still being investigated, but from what I've experienced, our healthcare systems don't have any effective treatments once people get to that point of their illness.
What these New York City care givers have had to endure is staggering. I get to help for a few weeks, but then I get to go home (where hopefully everyone is still crushing the curve, right?!?!?) and jump back in to taking care of trauma patients. The resilience of these providers is really where they have earned the oft-used title of "hero" in my book. It's one thing to jump in and help a patient or a teammate for a day, but to get up and do it over and over and over again is stunning.
From the frontlines – Day 14, NewYork–Presbyterian
This post was authored by Riley Chador, an RN at Primary Children’s Hospital, following her 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. Riley is deployed to NYP-Columbia University’s Hospital.
It’s easy to understand how care is sometimes dictated by fear. There are times I look at my patient and I am fearful. It’s easy to do when they’re lying in a bed, with a machine breathing in and out for them, tubes and lines everywhere. There’s no family around to remind you who they are. Sometimes when I look down at them and start to panic, I have to slow myself down and remember. It usually starts with touching their hand or rubbing their head. “Do you have children? We’re going to get you better so you can go home and see them.” I talk to them as I care for them because it helps me remember.
I talked to the most incredible nurse yesterday, the kind I would want to care for my family if they were here. She told me about how she motivates and encourages her patients. She gives them a daily pep-talk. Many of them have been intubated and sedated for weeks now. She brought up the point that many may think they’re going to die, that they don’t know they’re going to get better unless you keep telling them.
She spends her days talking to her patients. She tells them about their families. She tells them they’re waiting for them to come home. They’re ready. They’re so excited. They need to relax, rest, stop fighting the ventilator. Most of the time, once she starts talking about the patient’s family, she can see them visibly relax. Their heart rate goes down, their respiratory rate goes down— she’s able to hold off on that bolus of sedation.
It all makes sense. Usually family is a huge motivating factor. They put you at ease, they push you, and they help you do hard things. These patients are so sick and getting better is hard, it’s a lot of work.
I’m so grateful to be working with all of these amazing nurses—people that are much wiser than me both in life and in clinical practice. I’m learning so much from them. They take care of their patients and they take care of each other. They also take care of me; someone they have just barely met. They take time to teach me, set food aside for me in the break room, they rub my shoulder and encourage me on hard days. They’re incredible. These nurses and doctors are absolutely amazing.
Tuesday, April 28
From the frontlines – Day 14, Northwell Health
This post was authored by Janae Cheney, an RN at Layton Hospital, following her 2,200 mile journey to help caregivers in New York City. Janae is one of 50 caregivers deployed to help at Northwell Health and is at Long Island Jewish Medical Center in the emergency department.
When I made the leap to choose emergency nursing as a career, I never imagined I would be actively involved in working frontline medicine during a deadly pandemic. When it comes to the ER, there’s no such thing as predictable. Nurses thrive on the chaos and work exceptionally well under pressure. But the hardest part of being a nurse is when you have to play an active role in someone’s worst day.
When I accepted the offer to join the first crisis response team sent to New York from Intermountain, I had a mix of emotions and thoughts. I had a somewhat vague understanding of what we would be stepping into and experiencing. Now I see that every patient you see is having their worst day. That felt incredibly overwhelming. But I also knew that my nursing peers in New York, whom I’ve never met, needed help. That’s all I wanted to do by coming here, help support the nursing force, if even for a day.
I feel honored to work alongside these warriors, and I have learned a lot in a short period of time. It’s so challenging in a pandemic because we tend to hyper-focus on the medical aspect of things and the incredible amount of work, and sometimes the idea of humans caring for each other almost feels pushed aside. Our patients only see us in full protective equipment, we limit our time in their rooms, we turn away their family members. It’s a very tough environment. But they deserve to know that they have someone supporting them, and it's important to me they know that I’m that person.
From the frontlines – Day 13, NewYork–Presbyterian
This post was authored by Bengt Lock, an RN at Alta View Hospital, following his 2,200 mile journey to help caregivers in New York City. Bengt is one of 50 caregivers deployed to help at NewYork-Presbyterian and is at NY-Presbyterian Brooklyn Methodist Hospital in the emergency department.
I had today off so I decided I would take a break to do a little sightseeing. One of the other nurses came with me. We went on quite a trek. We walked across the Brooklyn Bridge and down to the World Trade Center Memorial. Unfortunately, the memorial and museum are closed but I was still able to see the large holes in the ground with the name plates. It was quite something. I was only 12 years old when 9/11 happened. I’m sure many of us remember exactly what we were doing, and on that day, I had faked sick so I could stay home from school. Luckily, my mom called me right after the first plane hit and encouraged me to watch the news. I remember my family watched the news for what seemed like weeks on end. And even though we weren’t able to fully experience the museum and memorial today, it was still very hallowed ground. To see the names written on the memorial was incredible. I’ve always wanted to witness it and I’m so grateful for I had the opportunity to come down and see it.
World Trade Center Memorial
While we were at the World Trade Center Memorial, I wanted to get a picture down into the pit where the water runs. I asked the security guard if he would take my phone and get a picture of me, but he said he couldn’t because my phone could have germs and that wouldn’t be following the rules of social distancing. They still are taking the rules very seriously — and I totally respect where he was coming from.
We then continued to walk down towards the Charging Bull and then to the waterfront to see the Statue of Liberty. From that point we walked up through a part of Chinatown and onto the Manhattan Bridge. It may sound nerdy, but I love seeing where a lot of the Avengers and Marvel movies have been filmed in New York City. (And let’s not forget the Spiderman movies as well.) There’s a scene in Avengers Infinity War where Spiderman, a.k.a. Peter Parker, quickly exits his school bus and flies under the bridge using his webbing and then goes into New York City. I made sure to stop on the bridge to try and get the same view that he had. Kind of fun knowing that Spiderman and I were on the same bridge! (HA!) It was quite fun to see all the sites.
While sight-seeing was a fun break, it’s definitely not New York right now because everyone is still socially isolating. The streets were extremely empty and very few people were out and about. There were hardly any boats in the harbor. For the most part it seemed kind of like a ghost town.
It’s nice to see how we as a society can come together for the greater good.
Monday, April 27
From the frontlines – Day 13, Northwell Health
Why are Intermountain pharmacist Brey Reachi’s thumbs so sore and what does that have to do with COVID-19? Deployed with team of caregivers supporting Northwell Health, hear from Brey’s perspective what it takes to adapt limited drug supplies to treat patients during a major pandemic.
Sunday, April 26
From the frontlines – Day 12, Northwell Health
Rachelle Rhodes, RN, MBA, Intermountain’s executive director of emergency department and trauma operations, was one of Intermountain’s administrative leaders who accompanied the COVID-19 response team to Northwell Health. The following is her perspective on leaders and leadership in a pandemic.
Reflections on Leaders & Leadership in a Pandemic: What Intermountain can learn from great leaders in New York
What does it take to make it through a pandemic? Let's talk about leaders and leadership. New York's Northwell leaders have been through tough events in the past. Think back on 9/11, Hurricane Sandy in 2012, and the recent “nor'easter” last week with 70+ mph winds that barely made the news in Utah. Well, as one individual said, “It was just a little windy.” These teams have had significant experience through events in their past to handle a pandemic and are examples to us all right now.
Making a new hospital
“No one ever had this plan in their books, though, it was a whole new beast,” said one leader. “This one stretched us all.” The environment changed so quickly and so dramatically that leaders had to respond immediately. Their goal was to stay ahead of the need by "one inch," or "20 beds," or "20 ventilators." They made decisions on the fly and implemented changes as they flew. One facility transitioned from five ICUs to nine ICUs in a matter of few weeks. They found beds in PACU units, transition or low acuity pre-discharge areas, and even auditoriums and medical libraries. They procured equipment as quickly as the beds were identified. One hospital reconstructed an open PACU area into individual rooms within five days – not with flimsy walls, but with metal studs, drywall, paint, doors – everything! Facility crews were magicians, they saw the vision and and created incredible places to work.
Leaders making it happen
But the remarkable thing about this pandemic is not just beds, new locations, or IV poles. The remarkable thing about this pandemic are the leaders. I saw a hospital executive who knows and loves her team so much she was rarely in her office because she was with her people. Donna Moravick of Northwell's North Shore hospital encouraged, listened, responded, and loved her team as we walked through her ICUs and auditorium care areas. People say “Hello, Donna” everywhere we went. “It's tough here,” Donna said as we walked through an ICU where they held two patients in each ICU room instead of one. Because the central monitor was set up for one per room, the decision was made to place one patient on the heart monitor and the other patient on the pulse oximeter so they could monitor both patients.
Alex Hellinger at Northwell's Greenwich Village facility is so embedded in his work that whenever I see this building, I will always think of Alex. He knows every square inch of this building and can tell you the Maritime history contained within. He has painstakingly preserved the spirit of the past and welcomed the technology of the future. He loves his people and his people love him. He doesn't ask anything of anyone that he is not willing to do himself. It is through these relationships that when he asked his people to do hard things, they followed. They've been scared, but they've followed. Greenwich Village was a free-standing ED and outpatient procedure facility until COVID helped them move to the next level - a community hospital. During this pandemic, they re-constructed their PACU into a medical COVID unit and then deployed outpatient physical therapists that assist with turning and ambulation. “We don't normally see the patient progress like this,” said one physical therapist. “Since we work in an outpatient setting, our patients come to us in a very different state than what we see here. I find it very fulfilling - we are making a difference!”
Driving hope
Whenever I hear the song, “Here Comes the Sun” it will remind me of the COVID pandemic. There has been so much death in these hospitals that refrigerated trucks were used as back up morgues. People would come to the hospital in respiratory distress and pass away within a few days or after lingering on a ventilator for a few weeks. It was a tough environment, and something needed to be done to provide some hope to the caregivers so they could continue caring for the sick patients. Often, patients didn't make it off the ventilator. But when someone became strong enough to get extubated, it triggered an overhead sampling of “Here Comes the Sun.” I sat in the Administrative Boardroom one afternoon after visiting with hospital leadership and heard that song seven times. Each time, I stopped, looked up and smiled. “Someone made it!” I prayed they would be able to remain off the ventilator and get well enough to go home. That surge of hope was enough of a reminder.
So, what does it take to make it through a pandemic?
What can Intermountain learn? It takes great leaders who love their people and where they work. It takes engaged and involved leadership who have a foundational knowledge of emergency plans, incident management and system coordination as well as municipality and governmental relationships and coordination. I believe Intermountain is on the right track. If we keep planning, preparing and practicing our emergency plans; if we work well with our local and government agencies; and most importantly, if we truly love our teams, know them personally, communicate openly, and celebrate successes along the way, giving hope to each other, we will be as prepared as an organization can be.
Rachelle Rhodes and Dr. RJ Bunnell touring New York City’s pandemic overflow facilities.
From the frontlines – Day 11, NewYork–Presbyterian
This picture and excerpt is from Dr. Amrapali Shah, a pulmonologist at Intermountain Medical Center. Dr. Shah is one of 50 caregivers deployed to help at NewYork-Presbyterian.
This is the CICU (cardiac intensive care unit) team that has been working with me the last 8 days. We had our first extubation today! One of the first things the patient laboriously wrote on her clipboard early this morning was, “Thank you all for your care” and “Bless you all.” One of our team members, an intern (front left) had COVID-19 and was out sick for 2 weeks. He calls every patient’s family every day and translates 3 dialects of Chinese for us. Many patients do not designate English as their primary language. So grateful for this experience.
Today, leaders at NewYork-Presbyterian took out an ad in Utah papers — including the Salt Lake Tribune — to recognize and thank our team in New York for their support.
Saturday, April 25
From the frontlines – Day 11, Northwell Health
Intermountain’s Dr. Dixie Harris, a pulmonologist at Alta View Hospital, shared her experience as a member of one of Intermountain’s COVID-19 response teams in New York with Business Insider. Based at Northwell Health's Southside Hospital in Bay Shore on Long Island, she's overseeing a full intensive care unit of severely ill, often younger, COVID-19 patients. In her interview, Dr. Harris described the resilience and loss on the pandemic's front lines in New York.
Business Insider article excerpts:
What’s it like in a COVID-19 ICU?
Inside the ICU, almost every patient is intubated, Harris explained. A few have come off ventilators and are still recovering before being transferred out of the ICU. Patients have been on more medications than she had initially expected. Some have four or five medications — from antibiotics to sedatives to blood pressure medications — being infused into the body constantly. The ICU has patients as young as in their 20s up through their 70s, she said. It's somewhat unusual to care for so many young people, and doctors feel extra pressure to find ways to help them recover. “For someone in their 40s, 50s, you want to try everything you can to get them to survive,” Harris said.
What’s the hardest part?
Inside, the ICU is silent without family allowed to be in the rooms with patients. “To me the thing that's the tragedy in this whole process is they don't have their family members there at the bedside," Harris said. Hospitals have limited visitors to help prevent the transmission of the coronavirus to otherwise healthy individuals. That's proved difficult because it's harder for staff to form the same relationship with families when providing updates on their loved ones as they might if the family was there in the hospital. And the conversations they're having, Harris said, are hard discussions.
"We want the families there, we just can't have them there," Harris said. Often, she said, the conversations are difficult because families haven't seen their loved ones in weeks by the time they're admitted into the ICU. They're not able to see the condition their loved ones are in, which can make having conversations about what to do next when patients aren't recovering even harder.
Looking ahead
“It's a fierce ongoing war,” Harris said. "It's clear this is going to be going on at these hospitals for a while. The thing that's surprised me the most are the attitudes of the staff. They're clearly not beaten.”
Read the full Business Insider article
From the frontlines – Day 10, NewYork–Presbyterian
This post was authored by Bengt Lock, an RN at Alta View Hospital, following his 2,200 mile journey to help caregivers in New York City. Bengt is one of 50 caregivers deployed to help at NewYork-Presbyterian and is at NY-Presbyterian Brooklyn Methodist Hospital in the emergency department.
Today has been a really good day. It seems that the emergency department is slowly getting back to normal, or at least what may be their “new normal.”
I had time to connect with an endoscopy tech* today and we had a conversation that really struck me. She had been relocated to the emergency department at the beginning of the COVID-19 crisis. We were walking out together at 7p.m. to see the fire trucks, neighbors, and others on the street cheering. In the midst of this celebration, of humanity at its best, we saw a hearse being loaded. This tech remarked on how she has been having nightmares for the past three weeks. In her nightmares, she is seeing people in body bags, over and over again. Can you imagine? She went from a job where nobody dies and you rarely have bad outcomes, to witnessing hundreds of deaths. There’s no way she could have ever been psychologically prepared to handle the things she has witnessed firsthand.
So, I did the only thing that I felt was allowed and appropriate at a time such as this. I gave her a half hug and told her she should be proud of herself. It seemed insufficient, but compassion and encouragement are all the tools available here right now. These are the real heroes! While the news talks about economic recovery of our nation, I was left wondering how these frontline heroes will recover from the complete devastation they have experienced firsthand. I know they have been in survival mode for weeks on end. I just hope these frontline heroes don’t get lost in society in the aftermath of the war against COVID-19.
Again, it’s these little moments that I experience every day that are so very humbling and remind me of how grateful I am that Utah has not been devastated like New York City. Here there are a few rooms designated for staff when they find they need a moment to regroup. I’ve heard of other health systems using tranquility rooms or tents. People from Intermountain have reached out to our teams several times already to check on us, assuring that we are both mentally and physically okay. Before we left for New York, emotional support was being offered by our organization in so many ways for anyone in our communities who may be suffering the effects of social isolation, loss of jobs, and financial worries. Our leaders have been proactive in setting up much needed support. I am so proud to represent our organization.
*A note for the reader: Endoscopy technicians are part of the medical team that use endoscopes to diagnose or treat gastrointestinal problems. They interact with patients, prepare the room and the equipment, provide support to physicians and nurses while the procedure is underway, handle specimens collected, and sterilize equipment.
Friday, April 24
From the frontlines – Day 9, NewYork–Presbyterian
Dr. Harland Hayes, an emergency medicine physician at Intermountain Medical Center, is one of the team leaders of the Intermountain team of caregivers deployed to help NewYork-Presbyterian. Harland is stationed at NYP-Columbia University’s Hospital in the emergency department—and experienced an unexpected surprise Wednesday morning.
The volume of patients in the New York City emergency departments (EDs) peaked a couple weeks ago, but there are still many sick, critically ill COVID-19 patients presenting for care. Because things have slowed down in the EDs, one of the gifts our emergency providers have provided is to fill in and staff the ER while the Columbia University ED doctors take some much-needed time off to recharge. This morning however, the ED was fairly busy.
At around noon, I had just finished putting a COVID-19 patient on a ventilator when we got the call that a woman in her late 20’s was being rushed into one of the ED resuscitation bays. The patient was in labor and things were moving quickly. Her water had already broken, and she was in a lot of pain. We changed our gowns and gloves and headed in to assess her.
It was apparent that there would not be time to move the woman up to labor and delivery; the baby was already crowning and wasn’t going to wait. I watched this brave soon-to-be-mom take everything in stride; it was definitely not the environment a young woman dreams of, delivering a baby in the emergency department during a pandemic. One of the nurses held her hand as another nurse began placing an IV and getting her on the monitors. Other nurses found a baby warmer, got it ready, and gathered medications and supplies. Again, this resilient team of Utah and New York nurses quickly adapted and focused on the patient in front of them.
This baby boy was determined. He’s not the first baby I’ve delivered (this happens every few years for me in the ED). Fortunately, this baby boy came quickly and without complication, and the mom did great. The baby perked up quickly, was vigorous and crying — a wonderful sign. I suctioned him, cut the umbilical cord, and passed him off to the nurses who got him under a warmer and stimulated him. Mom was stable with minimal bleeding. By the time the OB/GYN and pediatrician arrived, mom and baby were looking great.
At that point, the room was all smiles and congratulations. The mom was thrilled; she sat still and snuggled her newborn. The stress of a busy ED, the worries of a pandemic, and the pain of labor were behind her. She gazed through tear-filled eyes at her beautiful, perfect baby boy. After a short period, it was time for the OB team to wheel her up to the postpartum recovery area in the hospital. As they rolled the mom and baby through the emergency department, staff stopped what they were doing and applauded this woman and her new baby. It was a beautiful scene. This was a moment of renewal, of joy, and of hope in the midst of what is surely the most heartbreaking, trying season in this hospital’s history.
I’ll never forget this unexpected and sweet moment. It taught me once more that hospitals are sacred; human lives both leave and enter this world within the walls of these buildings. It’s a privilege to share these tender, difficult, and beautiful moments with patients and their families. Indeed, we were all touched to share this moment with this little family.
From the frontlines – Day 10, Northwell Health
This post was authored by Maranda Nelson, an RN in the ICU at Dixie Regional Medical Center. Maranda is one of 50 Intermountain caregivers deployed to help at two hospitals in the Northwell Health system and is based at Long Island Jewish Medical Center.
I've been helping out at Long Island Jewish Medical Center now for six of my ten shifts. The care teams celebrate everything here. Some days we hear the beautiful sounds of “Here Comes the Sun” playing over the hospital sound system (signifying a patient has been successfully extubated or discharged), some days we hear more rapid response or "code blues" called over the same speakers. While all this is happening, the New York nurses, doctors, RTs, PCTs, PAs, and NPs all make sure we know how grateful they are for our help. I've only been at this for a week and a half, they’ve been fighting forever it seems and still as strong as ever!
I've seen a lot during this time that I'll never forget. In my six days in one of the many ICUs here, I've seen multiple patients get better, then worse, and then slightly better again. I've seen the New York medical providers fight so hard to give the absolute best care every single day despite the long hours, days, and now months this effort has turned into for them. I've seen frustration, fear, anxiety, pain, exhaustion, joy, happiness, and relief wrapped up in a single day. I've watched everyone come together through a pandemic — incredible.
This experience has given me new skills and has allowed me to be a lot more patient with myself and others. It's allowed me to see the whole picture of medicine and physiologically what’s happening with the patient and it’s given me the knowledge and skills to know what to do with that information. More than that, it’s helped me see people on a deeper level and empathize more — it’s helped me see them as mothers, fathers, grandparents, and children.
I feel so lucky to be here working alongside so many wonderful, selfless people who flew out from Utah to help. The trust we've developed as a team, relying on each other professionally and emotionally, is more important now than ever. Hopefully I'll take what we've learned home to share with my team and help us prepare!
P.S. This morning I got a “You’re an Intermountain nurse, right? Thank God.”
Thursday, April 23
From the frontlines – Day 9, Northwell Health
Primary Children's Hospital nurse Jake Ferrin shares what it's like to treat pediatric patients with COVID-19. Jake is among Intermountain caregivers deployed to the Northwell Health Long Island Jewish Medical Center.
I just worked in the pediatric ICU at Northwell, they have an excellent team there. They're still reasonably staffed during the pandemic and have a good nurse to patient ratio. The pediatric world hasn't been hit by COVID like adult care settings, but they still had nine COVID patients last night and have lost two children on the unit since the pandemic began. It's heartbreaking.
I took care of a teenager on one of my shifts. He's been through a lot and was pretty delirious. He was previously intubated and put on a ventilator to help him breathe and had just been extubated and finally breathing on his own. We took him down to get a CT scan of his lungs and I was able to speak some Spanish with him and explain what was happening. While I was helping him to the CT table, I felt his hand and it was just burning hot from his relentless fever. You could tell how exhausted he was, your heart just goes out to kids who've been through all that and need to stay in the hospital for so long. I heard today that he was doing better — we'll take any progress we can get with COVID right now, it's a tough illness to treat when it gets this serious. Most intubated patients don't make it, but this kid is defying the odds.
The Northwell staff is great and you can tell they've been running so hard the past 5-6 weeks and giving 110%. They had me working as a "functional" or "resource" nurse to assist anywhere I could. Even though pediatrics isn't hit nearly as hard as the adult side, I took it upon myself if I had any down time to help these exhausted caregivers just for the sake of morale. It's so important to just talk to people. Connecting with them, trying to get them to laugh a little bit. To me, those small gestures help restore some humanity. Being able to help someone and put a smile on their face, even for a moment — to me those moments really empower all of us.
From left to right, Jake Ferrin, RN, Lindsay Paschal, RN, and Whitney Hilton, RN, getting ready to head out to their overnight shift supporting Northwell Health in Long Island, NY.
From the frontlines – Day 8, NewYork–Presbyterian
Shelly Wood, an Intermountain RN, explains the nightly 7:00 cheer the New York Fire Department leads for healthcare heroes, that takes place outside of the NewYork-Presbyterian Hospital she’s deployed to. “It brings tears to my eyes every night that I’ve been out here on the street for the end of my shift.”
Wednesday, April 22
From the frontlines – Day 8, Northwell Health
Zia Haider, respiratory therapist at Intermountain Medical Center, shares the outcome of two critical COVID-19 patients in the same ICU room and what caregivers are seeing every day in these settings. “You have people who don’t make it, but you also have people who are recovering. It gives you a glimmer of hope for patients.”
From the frontlines – Day 7, NewYork–Presbyterian
This post was authored by Riley Chador, an RN at Primary Children’s Hospital, following her 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. Riley is deployed to NYP-Columbia University’s Hospital.
The day goes on; you steady your shaky hands with tasks and focus your attention on the living. The people I'm working with are incredible: they're quick, adaptable, and resourceful. The ICU is a pretty dynamic environment with people calling things out in an already loud chaotic setting. It’s a crisis and you do what you can for yourself but also for others. The ICU doctors have been amazing. They're kind and patient. For example, they were out of the N95s I usually wear and one of the doctors couldn’t find one either. We ended up using a different brand for the day. Later, this particular doctor came and found me, tapping my shoulder while I was charting, and let me know she had found a few. She gave me two just in case I couldn’t find them again.
Today was a good day because I had a patient that may be extubated* tomorrow. I think all of us are pretty pumped about the possibility of extubating her. I also found oral swabs. It’s a small thing, but it’s so important to my nurse brain and heart. While you’re sick, paralyzed, and sedated you should get to be clean. That’s part of my job — to give you as much dignity as I can and to look after you because you can't look after yourself. It was a small win but that’s what I’m celebrating right now.
I'm on a team of incredible people and we're all learning as we do this. And at the end of the day, it’s a good day.
*A note to the reader: Sometimes, because of illness, injury, or surgery, you need help to breathe. Your doctor or anesthesiologist (a doctor who puts you to “sleep” for surgery) puts a tube (endotracheal tube, or ETT) down your throat and into your windpipe. Extubation is when a doctor takes out a tube that helps you breathe.
Tuesday, April 21
From the frontlines – Day 7, Northwell Health
This post was authored by Dr. RJ Bunnell following his 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. RJ is one of 50 caregivers deployed to help at two hospitals in the Northwell Health system in Long Island, NY.
Part of what we wanted to accomplish on this trip is learning everything we can in order to prepare for similar surges of patients back home. Utah appears to be on a different trajectory than New York as of now—but we cannot be unprepared.
I’d had a day off scheduled, but when my co-lead of this trip invited me on a guided visit to several care facilities in Manhattan, I had to grab a mask and go.
I’ve only been to New York City once before, and that was a month after 9/11. My only memories of downtown from that brief visit are at night; a deserted street in a canyon of towering buildings, muted silence, and at the end of the block, nothing but a black void and shrouds of dust still hanging in the air. Today was cloudy and chilly and the streets were deserted. For the length of Fifth Avenue, we marveled at a single car in the distance and maybe a handful of masked pedestrians. Central Park was greening everywhere with hardly anyone to see it. A block away, two refrigerated semi-trucks for bodies were parked behind the hospital. The trucks were parked across from multi-million-dollar brownstones, humming innocuously and covered partially by a tent that you’d see at an art fair.
We had the chance to visit a temporary medical facility in a sprawling convention center by the Hudson River that defied imagination. Even operating at a fraction of its capacity, hundreds of COVID-19 patients were being expertly taken care of by what was probably the biggest joint operation of any kind that I’d ever seen. Two branches of the military, state agencies, 3 health systems, and countless personnel have created a fully functioning hospital with an ICU where there had once been acres of empty concrete floors, only a week before.
The people from the system we have been volunteering at and the service men and women we interacted with today taught me a lot about selflessness and the power of collective action. I’m going to bed tonight profoundly grateful for having had the opportunity to witness the type of resourcefulness, dedication, and love that people are capable of when united by a common purpose.
From the frontlines – Day 6, NewYork–Presbyterian
I had the opportunity to round with the CNO (Chief Nursing Officer) at NY-Presbyterian Brooklyn Methodist Hospital today. From what I witnessed, there are many reasons why social distancing so very important back home.
NYC Brooklyn Methodist Hospital is similar to Intermountain Medical Center in numbers of patient beds and staffing. It’s a large hospital with over 590 beds. They usually have 34 ICU beds that now has expanded to around 125 ICU/vented patients. The psychiatric floor, 50 beds, was converted to an ICU with new negative pressure equipment added in it. The psychiatric patients were all transferred. The pediatric patients were moved to a different hospital and now, part of the pediatric unit was converted to a 10-bed COVID ICU and a 35-bed medical floor. There are only 190 private rooms in the entire hospital; the other rooms are all shared. The ED (emergency department) waiting room was transitioned to a mass patient room. Their ED patient visits increased from around 125 to more than 300 patients per day. They ran out of ventilators, so they have a ton of different types of rental equipment they are using in the ICUs. All elective surgery stopped on March 10. At the peak (April 5 - present), staff to patient ratios were 1:5 in the ICU, 1:12 in med floor, and 1:10 in the ED. Thankfully, all floors are moving closer to standard ratios, but it could change any day. The medical floors are 96% COVID positive patients. Almost 100 travel nurses have come in to support over the last few weeks to this hospital alone.

This hospital is averaging 10 COVID deaths per day since late March. They estimate that they have had 300 deaths from COVID at this hospital. Nearly all non-emergent or non-ventilated patients have been discharged or transitioned to an outpatient rehab center.
We don’t realize how good we have it right now. This was a great reminder of how fortunate we are in Utah and why we should continue to flatten the curve.
Monday, April 20
From the frontlines – Day 6, Northwell Health
Missy Best, an RN in the emergency department at Logan Regional Hospital, reflects on conditions in emergency settings at Northwell’s Southside Hospital in Long Island, amidst the COVID-19 outbreak. “You’re the safety zone for these patients,” says Missy.
From the frontlines – Day 5, NewYork–Presbyterian
Dr. Harland Hayes, an Intermountain emergency medicine physician at Intermountain Medical Center, is one of the team leaders for the team of caregivers deployed to NewYork-Presbyterian facilities. He received the following message from Dr. Erica L. Olsen, an emergency medicine physician at NewYork-Presbyterian Columbia, about the role Intermountain’s caregivers are playing in her life, personally.
Dr. Hayes and team,
THANK YOU.
I have been thinking of you throughout the entire weekend as I wrap my head around the generosity and selflessness that your trip to New York represents. I have seen many things in the past few weeks that make me just want to throw my hands up. . . But with what you’re doing, I really am humbled and I feel my heart is restored. The profound sense of goodness that you bring to the situation has me just in awe of you and I thank you truly for your spirit of partnership. I thank you for the fact that I can put my head down now tonight and know that I have space and time tomorrow to do some really simple things that have gone by the wayside and mean so much—get sleep, cook a healthy meal, call my parents and have a full conversation, play with my baby, and get outside. It’s such a gift that you are giving and I thank you sincerely. I will be appreciating my time off, that I promise. You’ve inspired me now to return the favor to someone else as this marches on. I hope that I get to meet many of you in person and thank you, but please know how very much your support is appreciated.
With gratitude,
Erica
Intermountain Medical Center ER physician, Harland Hayes, MD (red scrubs) with NewYork-Presbyterian ER caregivers.
Sunday, April 19
From the frontlines – Day 5, Northwell Health
This post was authored by Whitney Hilton, an RN at McKay-Dee Hospital, following her 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. Whitney is deployed to Northwell Health’s Long Island Jewish Medical Center.
This is a humbling experience. I have so much to say but almost too overwhelmed to say it all. New York has been hit HARD. The people need help, the nurses need help, the doctors need help, everyone needs help. This is crisis mode like I’ve never seen. This is an incredible experience, albeit the hardest thing I’ve ever done AND equally the most rewarding.
Another day in the ICU here in New York. Today was considered a “slow” day for these nurses & doctors, which honestly is almost comical at this point. But I guess anything less than an absolute crisis is a good day to them. I’m trying to give you all a real picture of what it’s like here because this isn’t about ME; this is to show you how REAL COVID-19 is & how SCARY it is. We are SO incredibly blessed in Utah and slowly the spread is the only way to keep us safe.
One thing I want to SCREAM from the rooftops is that if you could see what we see here, you’d do ANYTHING humanly possible to prevent it.
- We had a patient code and die today. It was incredibly sad to witness, and I pray for the patient’s family that couldn’t be there. I hope they know that we held the patient’s hand as he passed. The teamwork involved was so powerful! Nurses and doctors coming together & risking their health to save someone was amazing to be a part of.
- Because these patients’ families aren’t with them when they pass away, the nurses are hand making the families a little card with a fingerprint of the patient and an EKG strip (heat rhythm).
- The nurses are burned out; they've been through these last couple of weeks.
- If your family member is hospitalized, having pictures for them in the room is so helpful for the patients and the staff, so everyone can remember that they are more than just patients—and deserve the utmost care.
- This is a modern war.
- With each passing day and shift I work, I’m so grateful for the opportunity to be here helping these New Yorkers.
- I can proudly say I drove around in New York City without any traffic.
A picture is worth a thousand words. Meet Libbey Steed, an RN at Dixie Regional Medical Center, deployed with our Northwell Health team. This is Libbey after her shift — 12 hours in an N95 mask.
From the frontlines – Day 4, NewYork–Presbyterian
This post was authored by Riley Chador, an RN at Primary Children’s Hospital, following her 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. Riley is deployed to NYP-Columbia University’s Hospital.
I am working at NYP-Columbia University’s campus, a 2,600-bed hospital with (normally) about 117 dedicated ICU beds— currently at around 260 ICU beds. The campus is immense and especially beautiful this time of year, with blooming trees and quiet manicured gardens. There are of course less pleasant scenes; the tents set up outside of every ER, the line of ambulances backed up from the bay all the way down the street, and the trucks. The trucks are what probably shook me the most.
Mostly, I am awestruck. People are rising to the occasion. In a time of fear, suffering and isolation, the medical community and New York City have come together and rallied in incredible ways. There is a 288-bed world class field hospital set up and fully staffed by active military members and veterans to lighten the load on hospitals. At NYP, they have turned OR’s into 85 ICU beds and are placing multiple patients on the same ventilator. I see kindness, encouragement and camaraderie everywhere I turn. People walking down the street say thank you, there are signs on windows, words of encouragement on the sidewalk, and at 7 p.m. the eerily quiet city goes wild. The 7 p.m. cheer is what they call it. Firefighters and engines gather outside of the hospital honking their horns, church bells ring, people scream, shout, cheer and bang pots and pans. They’re thanking us and they’re thanking each other.
Photo of refrigerated trucks being used as temporary morgues in New York City.
Saturday, April 18
From the frontlines – Day 4, Northwell Health
This post was authored by Dr. Jarid Gray, a hospitalist at Cedar City Hospital, following his 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. Dr. Gray is deployed to Northwell Health’s Long Island Jewish Medical Center.
Back to Long Island Jewish Medical Center for another day helping New York’s COVID-19 response. Today I was given my own, albeit abbreviated list of patients to manage independently as I continued to learn the workflow and computer system. I learned that another patient we saw yesterday had passed in the night. All of today’s patients were on our list from yesterday, so at least I had some familiarity with them.
After a quick pre-round, I donned my N95, a surgical mask over the top of the N95, goggles, and face shield. All of the patients that I cared for today were COVID-19 positive. Two of them were worse off than the day before. We placed them on their stomach (proned them) in attempts to improve their oxygenation. Both of these patients stabilized following this maneuver, staving off intubation for at least a day. Thankfully, the overhead calls were significantly reduced, having only 10 calls for rapid response throughout the day.
At the end of our shift, the FDNY lined up their fire engines near the employee entrance/exit and clapped and cheered for the caregivers as they either arrived or were finishing their shifts for the day. It was a touching gesture from them, and it gave me chills watching it happen.
Tonight, the Intermountain team held a debriefing at the hotel to review the day’s events. As it was wrapping up, I reflected back on the last two days. The more I digest what’s happening, the prouder I am of our team and my profession in general. Despite going up against what seems to be an unbeatable disease, that could potentially infect any of us, we still rise to the occasion. We run towards danger to help others. Even when we are beaten down, we wipe away the tears, dust ourselves off, and defiantly rise for another round. We enter each room, see each patient, will a steeled determination to make a difference for that patient, for that family who cannot be there, desperate to hear any good news from us. We search for novel treatments; others search for an effective and safe vaccine. To steal a line from Winston Churchill… “We shall fight for our patients, we shall fight on the laboratory bench, we shall fight in our communities and in the dark corners of our society, we will never leave anyone behind or allow anyone to die alone; we shall never surrender.” I love my profession, I love my job, and I love the company that I work for.
From the frontlines – Day 3, NewYork–Presbyterian
This post was authored by Fernando Rivero, an Intermountain emergency medicine PA, following his 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. Fernando is deployed to NYP’s Allen Presbyterian Hospital.
Day one is done. Three of us worked at the Allen Presbyterian Hospital; it is northern part of Manhattan Island bordering the Bronx. It is a place that has gotten hit the hardest. It’s a small 25 bed community Hospital. Last week they had over 100 patients in the ER at one time. They currently have about 50 — about a dozen on ventilators waiting to go to the ICU, and unfortunately for some of them, waiting to die. We feel very appreciated and well utilized. It is very humbling. We are received daily with unnecessary applause and cheers and a lot of gratitude from everybody including the staff that we are here to help, for just doing our jobs. Every patient I saw today had COVID-19. We are wearing a respirator mask and goggles for 12 hours daily. I took my mask off over two hours ago but I still have the outline of the goggles on my face. You eat and drink at the beginning of the shift, and then not again till your shift ends. Removing the protective equipment puts you at risk of contamination. Two hours later I can still see the lines on my face from the goggles. I think of the people who have been wearing them for weeks and weeks, and wonder if their faces will always be marked, if our faces will be marked, to remind us of this tragic day.
The NYC providers are worn out. Many of them are sleeping in the hospital, at least up until recently, because they are afraid to go home out of fear of contaminating their children and families. The nurses, the housekeepers, the people making food in the hospitals, and so many others are the true heroes, and they are exhausted. We only hope we can give them a very slight respite. Every day you come out of the hospital, people clap for you and cheer and all say thanks. It’s a little uncomfortable but very, very humbling.“
Friday, April 17
From the frontlines – Day 3, Northwell Health
This post was authored by Dana Chapman, RN in Layton Hospital emergency department, following her 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. Dana is deployed to Northwell Health’s Long Island Jewish Medical Center, in the emergency department.
"I'm working in the ED (emergency department) right now and pretty much every patient is considered a possible COVID patient. We don full PPE (personal protective equipment) most of the time. These New York nurses definitely have the process down—they’ve had so many patients, you have to really try to keep up with them! The biggest thing we're helping with is being that extra set of hands that knows what they're talking about and knows what they need, like I.V.s, drawing labs, and giving meds. It's been an amazing experience. Their hospital staff has accepted us with open arms and are willing to help us with anything. No question is a stupid question and I have a lot of them. Everyone is so incredibly supportive of us being here… they’ve been through a lot.
While a big surge in cases hasn't happened in Utah yet, my advice for everyone is to just be diligent. Act like it has. The better we are at following these strict PPE guidelines, the safer we'll keep ourselves, our families, our patients—everyone.”
From the frontlines – Day 2, NewYork–Presbyterian
The following entries were authored by caregivers deployed to three NewYork-Presbyterian hospitals. After arriving in New York yesterday, the team has gone on walk-throughs of the facilities and participated in orientation. Their first day in units will be tomorrow.
Kim Di Ciolli, RN, Intermountain Medical Center emergency department: “I’ve been to New York before and it’s weird how quiet it is. One example is from the airport to our hotel, it only took about 30-45 min. Typically in New York, that would be a few hours. In Manhattan, there is a little activity but nothing like I remember from my trip 4 years ago. You’re not bumping shoulders per say. For those of us staying in New Jersey, they have strict stay at home orders. Parks are closed as well as shops, and the bridge to New York closes at 8 p.m. (curfew is from 8 p.m. - 5 a.m.). You have to show your badge for proof you are an essential worker. I am at the NewYork–Presbyterian Columbia campus; the buildings are beautiful in brick. The team has been incredibly warm and welcoming. They have shared how they had changed the infrastructure in the hospital to accommodate the critically ill patients, like starting at 117 ICU beds to now 258 ICU beds. They converted the OR, cath lab, and Med surg units. It’s been surreal. I feel excited and ready to help ease the load. I am humbled by their efforts already and feel honored to be able to work alongside them and hopefully can help relieve the nurses and techs.”
Nathan Barney, RN, Primary Children’s Hospital PICU: “I think a common thing we all agree on is that while we may be getting recognized as “heroes,” we’re nothing compared to the caregivers who have been here fighting for the last month. The flexibility, the resolve. . . it’s incredible.”
Barb Ziegler, nurse practitioner, LDS Hospital: “I am in awe of what’s taking place inside these walls. The quiet streets, the locked doors at the nail salon, and the tape on the floor in the hotel lobby that marks the distance we must stand apart only tells part of the story. The other part—inside these walls—is the ENT physician who has learned how to insert an arterial line and manage vasopresors; the strong, burley orthopedic OR nurse who is now a part of the ICU proning team; the ICU nurse-to-patient ratio that’s 8:1 on a good day, and 12:1 on a not so good day. We’re all in this together. Just because we have to stand apart to be safe, we also have to stand together to be safe.”
Thursday, April 16
Intermountain’s second team of caregivers for the COVID-19 response team left Salt Lake City today and arrived in New York to assist three hospitals and caregivers apart of NewYork–Presbyterian. The 45 member team picked up their gear and received orientation at the Employee Services Center yesterday. Here’s what a few of them had to say about this deployment.
From the frontlines – Day 2
This post was authored by Dr. Dixie Harris following her 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. Dixie is one of 50 caregivers deployed to help at two hospitals in the Northwell Health system in Long Island, NY.
Today was my first day working with the caregivers at Southside Hospital in Long Island, New York. Speaking with the driver on my way to the hospital, I learned about his fellow driver, a 40 year-old father of two young children, who died from COVID-19. A sobering, yet realistic start to the day that illustrates how this disease is impacting the community.
Upon arrival to the hospital, we went through a familiar process of getting an orientation, being brought up to speed on the plan for the day, receiving my badge, getting access to their computer system, and reviewing their ICU protocols for how to treat all these COVID-19 patients in desperate need for help. While waiting for an ID badge, I listened to friendly banter of security, staff, and visitors. I overheard a conversation about how although they’ve seen a lot of deaths at their hospital, they haven’t resorted to “stacking bodies,” like what’s being reported in Detroit.
Once on the unit, we witnessed the overwhelming number of extremely critically ill patients. I learned about their “proning team.” Northwell implemented these teams around Easter; their sole responsibility is to turn patients over onto their belly, then flip them back into the supine position for shorter periods of the day. Preliminary information indicates that patients in the advanced stages of this illness seem to do better while lying on their stomach. With so many COVID-19 patients to care for, it takes a dedicated team to make this happen as quickly as possible.
I joined the head of ICU, Dr. Silverstein, and toured the medical COVID-19 ICUs. I met several ICU teams, participated with rounds discussions including how to successfully extubate patients, coding decisions, and medical futility.
Overall, the calm and pleasant demeanor of the Northwell hospital staff and doctors in the setting of unprecedented crisis is inspiring. As I observed their clinical rounds, there was an atmosphere of teamwork with respectful and open discussion. Although there was a significant amount of work to do, everyone I met stopped what they were doing and immediately expressed gratitude for the Intermountain team coming to New York to help.
At the end of my shift, I returned to the hotel and took a relaxing walk and reflected on the day. I joined our team in the lobby and looked out on this dedicated group, all masked, all preparing each other for their first day on the floor to fight this disease alongside the brave caregivers from Northwell Health. Calm and ready for another day.
VIDEO: Mark Solazzo, Executive VP and COO at Northwell Health in New York expresses his gratitude for the Intermountain COVID-19 response team.
Wednesday, April 15: Day 1 - From the frontlines
This post was authored by Dr. RJ Bunnell following his 2,200 mile journey to help caregivers in New York City, the current epicenter of the COVID-19 pandemic. RJ is one of 50 caregivers deployed to help at two hospitals in the Northwell Health system in Long Island, NY.
A message from RJ Bunnell, MD, Medical Director, Care Transformations
“The team was treated like conquering heroes today. Right off the bat we had Paul Krakovitz and Heather Brace, two of our senior leaders, at the airport security entrance wishing us well. The gate agents announced us and clapped. The flight crew made us the reluctant stars of our own half-empty plane. The Northwell staff who met us at the hotel couldn’t have been warmer or more professional. Travel today was by no means normal, but it was really touching and humbling to be recognized by so many total strangers for something that we’d volunteered to do. I knew it already, but it’s never been clearer to me that I work with truly exceptional people. The kind of people who run towards danger and will knock down the door to get into the burning building to help.
It’s obvious the toll this virus has taken on the community. People are tired. The streets are half empty and there is an eerie quiet outside of my hotel window. There are masks and sanitizer and people clumsily trying to keep an appropriate distance from each other everywhere. It’s clear from talking to their COO and Chief People Officer at Northwell Health that this crisis has stretched them to the limit, and also brought out the best in their people. At one point in the last month they were adding 200 beds a day to keep up with the new COVID-19 patients coming in every day. Their system is now operating with a thousand more patients than their worst-case projections. In a matter of weeks their hospitalist service at Long Island Jewish Medical Center went from 240 patients to over 600! 85% of the patients in their entire system have the virus. Deaths are a common daily occurrence and the RRT and Code Blue calls that used to average 90/month are now happening 20 times a day. Progress is incremental. While at first only 10% of intubated patients were surviving, now 40% are eventually able to breath on their own and come off the ventilator. A line from “Here Comes the Sun” by the Beatles plays on the hospital PA system when COVID-19 patients are discharged alive. What a beautiful anthem of hope in such dark times! We’re entering the “hot zone” tomorrow, and we can’t wait.”
Intermountain's COVID-19 Response Team after completing orientation at Northwell Health.
Intermountain caregivers share their "why" behind choosing to go to New York.
Tuesday, April 14: Preparing for deployment
The first team of caregivers from Intermountain Healthcare's COVID-19 Response Team left Salt Lake City today to assist hospitals and caregivers in New York who are on the frontlines of the COVID-19 pandemic. The 50 member team is headed to Northwell Health in New York and stopped by the Employee Service Center for orientation and gear pick-up. Here’s what some of them had to say about choosing to go on this deployment.
From Cheyanne Flores, RN at McKay Dee Hospital: “It was really nice that Intermountain was able to put this together so quickly. And I’ve been really proud to say I’m going with Intermountain as a deployment to help. That’s kind of the goal when you’re a nurse. You want to help, in anyway you can, so this is my dream come true. When I’m able to go get there and help the nurses specifically, I want to be able to take that load off their shoulders — whether they can teach me something to help them or if I can give them a day off and work a little extra. I’m willing to do that; I’m fresh, I’m ready. I’m there to help fight the fight.”