In an interview with KSL Radio this week from the AHA’s scientific sessions in Anaheim, Intermountain’s Dr. Anderson suggests watching your blood pressure closely.
“I think you should start to worry if it’s over 120 and get on to lifestyle changes,” he said. “Certainly if it’s over 130, you ought to be working with your healthcare provider and your physician to make sure you’re going to get that down over the long term.”
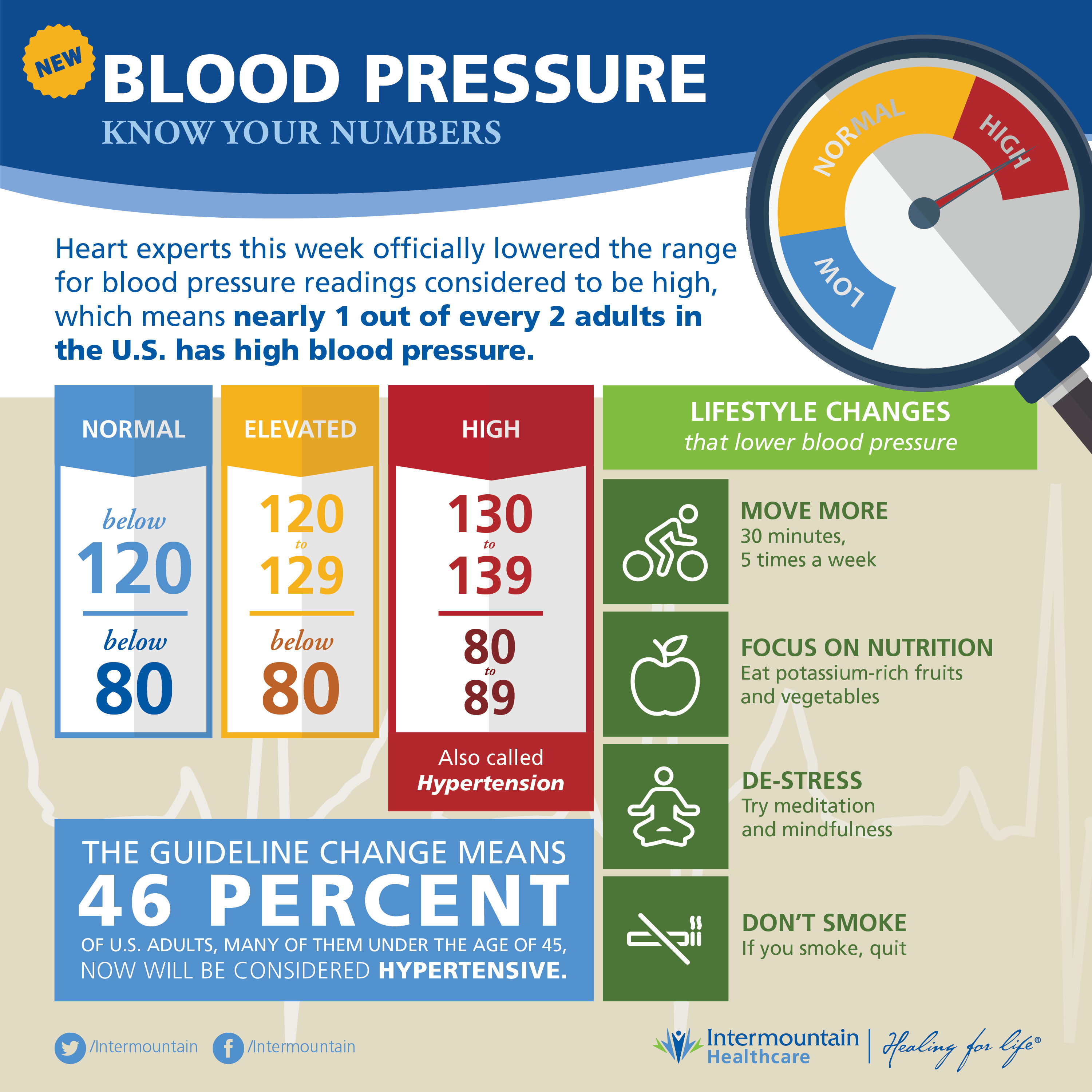
Instead of recommending drug treatment right away, the organizations that issued the new guidelines hope that many people found with the early stages of the condition will be able to address it through lifestyle changes such as losing weight, improving their diet, getting more exercise, consuming less alcohol and sodium, and lowering stress.
Dr. Anderson agrees: “Diet and exercise can have a tremendous impact, so that’s the first place to start.”
Additional examples of blood-pressure lowering lifestyle changes are in the infographic above, courtesy of CardioSmart.)
“This is a wonderful advance to help all of us reduce the risk of stroke, heart attacks, and heart failure, which really are three out of the top five or six reasons that as we get older we have significant disability and mortality associated with our lifestyle,” said Dr. Anderson.
High blood pressure damages blood vessels and can lead to organ damage such as kidney and heart failure, as well as heart attacks and stroke. It’s one of the leading killers around the world as well as across the United States.
While people may be confused by the change, the heart experts said three years of reviewing the research showed that many fewer people die if high blood pressure is treated earlier.