Perhaps because of its apparent simplicity, implant-based reconstruction is a commonly-chosen option for breast reconstruction among mastectomy patients. For the vast majority of women, an implant-based reconstruction can be divided into two steps: tissue expansion and permanent implant placement. In your clinic appointment, ask to see a sample of a tissue expander and an implant to help you visualize the process of reconstruction.
The placement of a tissue expander (a temporary, adjustable implant) is ideally performed at the time of mastectomy, but in many cases may be performed after a woman has healed from the mastectomy. The tissue expander is placed below the pectoralis major, a muscle of the chest.
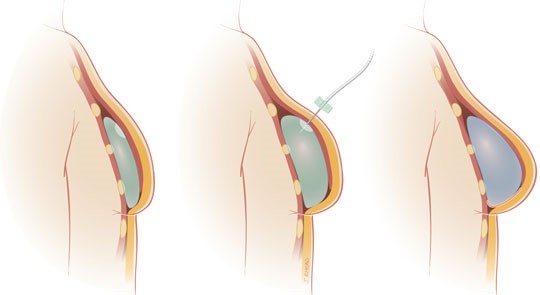
Because the chest muscle is not in the shape of a breast, it is necessary to undergo a shaping or expansion phase. A biologic form (such as Alloderm) may be used to help create shape of the lower portion of the breast and define the new breast fold. The expander itself is an empty sack with a medical tube called a port. Saline (salt water) is pumped into the expander via the port to increase its volume. In order to minimize pain and prevent tissue damage, saline is added a little at a time, every week or two until the appropriate volume is reached. Once the goal volume is achieved, the expander is left in place for a minimum of four months. This reduces any recoil of the tissues. Then, in an outpatient procedure, the expander is removed and a permanent implant of comparable size is inserted to replace it. This can typically be done through the already-existing mastectomy scar.
Benefits of an implant-based breast reconstruction may include a shorter operative time, a shorter hospitalization (if any at all), no donor site, and faster initial recovery. The general disadvantages of implant-based reconstruction may include less natural ptosis (the term for how the breast slopes on the chest), implant infection, implant rupture, capsular contracture, and frequent clinic visits during the expansion phase.